WASHINGTON, DC—While the VA significantly lags behind other healthcare systems in mandating influenza vaccinations for healthcare workers, according to recent research, it is moving closer to the national average because of a directive issued last fall.
That directive led to a nearly 40% boost in immunization rates among VA providers, according to the health care system.
The study in JAMA Network Open found that 61.4% of U.S. hospitals required influenza vaccinations for their healthcare staff last year, up from 37.1% in 2013. That represents a more than 50% increase in facilities mandating vaccinations. Among non-VA hospitals, the number requiring vaccination against influenza rose from 44.3% to 69.4%.1
That contrasts with just 4.1% of VA hospitals mandating influenza immunizations for healthcare personnel (HCP) in 2017, a statistically insignificant increase from the 1.3% reported in 2013, according to Greene and his colleagues.
“In just four years, the non-VA hospitals have really stepped up on requiring the vaccine, rather than just encouraging it,” explained M. Todd Greene, PhD, MPH, an epidemiologist at the VA Ann Arbor Healthcare System and an assistant research scientist in the Division of Hospital Medicine at the University of Michigan Medical School. “Studies have shown that vaccination mandates, coupled with an option of declining vaccination in favor of wearing a mask, are most effective in reaching high percentages of vaccination.”
The study compared results of surveys sent to hospital infection preventionists every four years. The 2013 data included 463 hospitals, of which 31 were VA facilities. In 2017, 599 hospitals participated, including 30 VA facilities.
Requiring influenza vaccinations significantly boosts immunization rates among healthcare workers. An earlier study by Greene and his colleagues at the University of Michigan, published in Infection Control and Hospital Epidemiology this spring, determined that mandates increased vaccination rates by up to 30%. The study compared influenza vaccination rates at three university medical centers that required immunization of healthcare workers to four VAMCs that did not.2
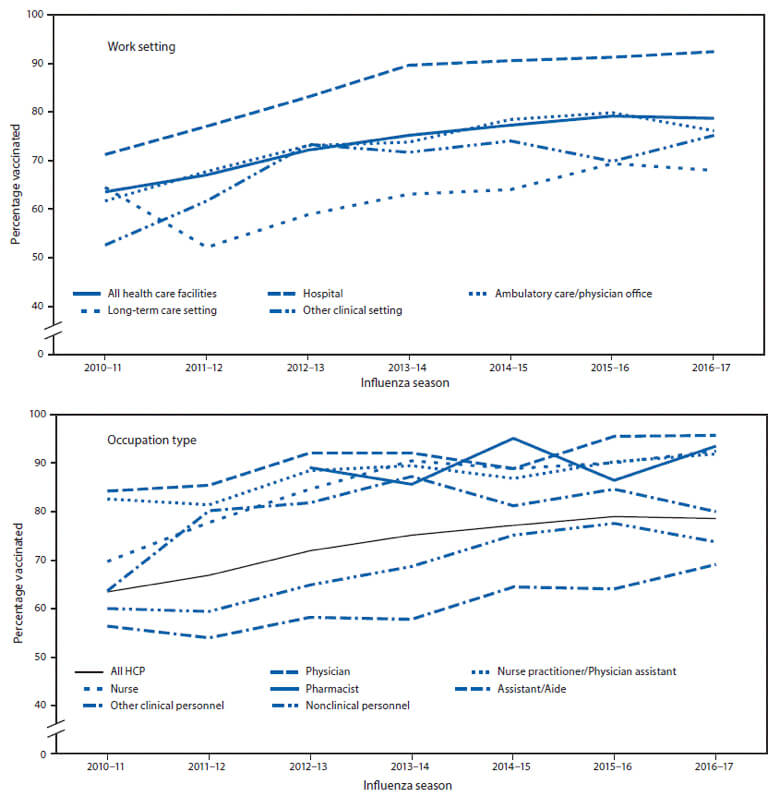
Facilities that require influenza vaccinations for healthcare workers have immunization rates above 96%, according to the national Centers for Disease Control and Prevention (CDC). That’s substantially higher than the overall influenza vaccination rate among healthcare personnel. During the 2016-2017 influenza season, the most recent available, the CDC reported that 78.6% of healthcare workers received the flu vaccine. That percentage has remained relatively constant for several years, at 77.3% in 2014-15 and 79% in 2015-16.3,4
At the VA, the vaccination rate has been less than two-thirds the national average—and well below goals set by government and accrediting organizations. In fiscal year 2016, healthcare workers at the VA had a seasonal influenza vaccination rate of just 50%, according to VA spokesperson Curt Cashour.
The CDC’s Advisory Committee on Immunization Practices recommends annual vaccination against influenza for all healthcare “personnel in inpatient and outpatient care settings, medical emergency-response workers, employees of nursing home and long-term care facilities who have contact with patients or residents.” The U.S. Department of Health and Human Services has set a Healthy People 2020 goal of a 90% influenza vaccination rate for healthcare workers.
“Beginning fiscal year 2013, VA health care facilities were expected to align their influenza vaccination for health care personnel with this goal. Facilities will need to look at their vaccination rates for the previous year and set a goal to increase which will meet the Joint Commission [and] 2020 Healthy People objectives,” according to the goals for the 2018-2019 VA influenza vaccination program. The Joint Commission adopted a standard of 90% in 2012 and requires facilities to document progress toward this goal.
The VA’s 2016 vaccination rate was also below the national baseline of 55.8% measured in the 2010-11 National Health Interview Survey which was used to set the 2020 goal.
To increase vaccination rates among healthcare workers, Poonam L. Alaigh, MD, the VA’s acting undersecretary for health, issued an immunization directive last September. The directive stated that “voluntary HCP influenza vaccination programs, including VHA’s, have been largely unsuccessful in achieving increased vaccination rates” and that “policies mandating influenza vaccination of HCP are supported or endorsed by many leading professional healthcare consumer organizations.”
Still, the directive did not mandate influenza vaccinations. Instead, it required all VA healthcare personnel to “receive seasonal influenza vaccination annually or to wear a mask throughout the influenza season” in most clinical and nonclinical areas, as well as outside of medical facilities when they would be in contact with VA patients. Healthcare workers need to receive and document vaccine receipt by November 30 each year or sign a form agreeing to wear a face mask.
As a result of the directive, VA healthcare worker influenza vaccination rates rose to 69% for fiscal year 2017, according to Cashour, representing a 38% increase.
“VHA will continue to promote vaccination through a variety of methods, distribute best practices, monitor and evaluate facility vaccination,” he added. “It is expected that the vaccination rates will continue to increase this season.”
The VA results align with Greene and his colleagues’ finding that having a written policy in place and encouraging vaccination can raise rates. So can transparency. Greene noted that hospitals that participated in the Hospital Quality Reporting Program had a more than 90% vaccination rate. The program requires hospitals to report the percentage of their healthcare workers who have received influenza vaccines each year, and the results are posted online.
1. Greene MT, Fowler KE, Ratz D, Krein SL, Bradley SF, Saint S. Changes in Influenza Vaccination Requirements for Health Care Personnel in US Hospitals. JAMA Network Open. 2018;1(2):e180143.
2. Greene MT, Fowler KE, Krein SL, Gaies E, Ratz D, Bradley SF, Saint S. Influenza Vaccination Requirements for Healthcare Personnel in U.S. Hospitals: Results of a National Survey. Infect Control Hosp Epidemiol. 2016 Apr;37(4):485-7.
3. Black CL, Yue X; MPS, Ball SW, et al. Influenza Vaccination Coverage Among Health Care Personnel – United States, 2016-17 Influenza Season. MMWR Morb Mortal Wkly Rep. 2017 Sep 29;66(38):1009-1015.
4. Black CL, Yue X, Ball SW, et al. Influenza Vaccination Coverage Among Health Care Personnel—United States, 2015–16 Influenza Season. MMWR Morb Mortal Wkly Rep.em> 2016 Sep 30;65(38):1026–1031.

