NEW YORK — New research is raising questions about whether the VA is doing enough to promote influenza vaccination of healthcare personnel.
The research compared three university medical centers with mandatory influenza vaccination policies to four VAMCs where flu immunization was not required at the time of the study.
Results were published in the journal Infection Control and Hospital Epidemiology. The study team, including researchers from four different VAMCs, demonstrated that mandatory flu vaccines for healthcare personnel (HCP) improved vaccination rates by as much as 30%, while reduced absenteeism during high-demand periods by about 6%.1
In addition, vaccinated healthcare workers had a 30% overall reduction in absenteeism compared with nonvaccinated healthcare workers overall. That information has increased significance with sky-high hospitalization rates for the flu season just ending. The national Centers for Disease Control and Prevention reported at the end of March that, since Oct. 1, 2017, 27,438 laboratory-confirmed influenza-associated hospitalizations had been reported through the Influenza Hospitalization Network (FluSurv-NET), a population-based surveillance network for laboratory-confirmed influenza-associated hospitalizations. That translated to a cumulative overall rate of 96.1 hospitalizations per 100,000 people in the United States—one of the highest ever documented with the flu.
“Our findings have implications for healthcare institutions, governmental agencies and others whose goal is to provide the safest work environment,” the authors wrote. “This study suggests that mandatory vaccination policies were associated with increased HCP vaccination rates and with reduced occurrence and duration of symptomatic absences. Reducing symptomatic absenteeism among HCP could help maintain the staffing and functioning of healthcare organizations during patient surges, including those occurring in an influenza epidemic.”
The report noted that both the Advisory Committee on Immunization Practices [ACIP] and the Hospital Infection Control Practices Advisory Committee [HICPAC].recommend that HCP without medical contraindications receive the influenza vaccine annually. In addition, it pointed out,” more than 600 professional organizations, healthcare systems, cities, states and federal agencies now mandate influenza vaccination for HCP. Mandatory vaccination policies substantially increase rates of HCP vaccination. However, HCP acceptance of voluntary vaccination continues to be problematic.”
The Influenza Action Coalition currently has more than 660 U.S. healthcare systems on its “honor roll” for mandating flu vaccination.
The retrospective observational cohort study was conducted at three university medical centers—Denver Health Medical Center, Children’s Hospital Colorado in Aurora and Johns Hopkins Health System in Baltimore—as well as four VA facilities—VA Eastern Colorado Healthcare System in Denver, Michael E. DeBakey VA Medical Center in Houston, DCVAMC in Washington and VA New York Harbor Healthcare System. At all locations, healthcare works were offered free, onsite vaccinations.
In total, the study included 2,304 outpatient healthcare professionals at mandatory vaccination sites and 1,759 outpatient HCP at nonmandatory vaccination sites. HCP participating in the Respiratory Protection Effectiveness Clinical Trial (ResPECT) at both mandatory and nonmandatory vaccination sites over three viral respiratory illness (VRI) seasons (2012-2015) reported their influenza vaccination status and symptomatic days absent from work weekly throughout a 12-week period during the peak VRI season each year.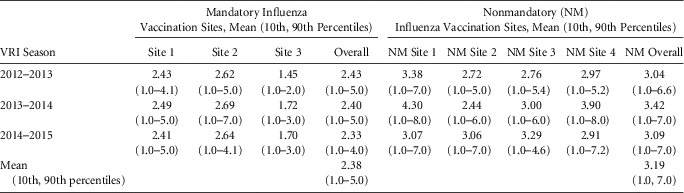
Results indicated that the proportion of participants who received influenza vaccination was lower each year at nonmandatory than at mandatory vaccination sites (odds ratio [OR], 0.09; 95% confidence interval [CI], 0.07-0.11).
Lower Absenteeism
In addition, among HCP who reported at least one sick day, vaccinated HCP had lower symptomatic days absent compared to unvaccinated HCP (OR for 2012-2013 and 2013-2014, 0.82; 95% CI, 0.72-0.93; OR for 2014-2015, 0.81; 95% CI, 0.69-0.95).
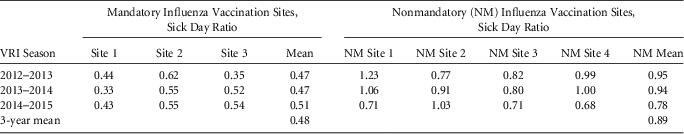
“These data suggest that mandatory HCP influenza vaccination policies increase influenza vaccination rates and that HCP symptomatic absenteeism diminishes as rates of influenza vaccination increase,” study authors concluded, adding, “These findings should be considered in formulating HCP influenza vaccination policies.”
Last fall, Poonam L. Alaigh, MD, acting under secretary for health at the VA, issued a directive for the Seasonal Influenza Prevention Program for VHA Health Care Personnel, which fell short of requiring mandatory influenza vaccination for HCPs.
“To prevent and control seasonal influenza and its associated complications, the Veterans Health Administration (VHA) requires a policy and implementation guidance that will ensure VHA achieves the Department of Health and Human Services (HHS) Healthy People 2020 goal and The Joint Commission standard of annual seasonal influenza vaccination of 90% of health care personnel (HCP),” the directive stated, adding, “This directive articulates the VHA policy requiring all HCP to participate in the seasonal influenza prevention program and outlines the key implementation steps. HCP covered by the policy are expected to receive annual influenza vaccination. Those HCP unable or unwilling to be vaccinated are required to wear a face mask throughout the influenza season.”
According to the document, the policy will stand until it is scheduled for recertification on or before the last working day of September 2022.
The directive dictates that, by Nov. 30 each year, HCP as defined in this directive must sign and submit to the facility Employee Occupational Health staff the Health Care Personnel Influenza Vaccination Form to indicate whether they have been vaccinated and provide necessary documentation if they have been vaccinated elsewhere. If they opt to refuse vaccination, they must acknowledge that they have read, understood and agree to comply with the requirement that they will be expected to wear a face mask throughout the influenza season.”
Not Liking Needles
On the form, reasons for declining vaccination include not liking needles, having a philosophical or religious reason for declining the vaccination, allergy to the vaccine or one of its components, concern after the side effects or safety of the vaccine, that he or she has never had the flu and doesn’t think it will be an issue this season or another, unspecified reason.
A similar policy recently was challenged at a prestigious medical center. The Massachusetts Nurses Association is suing Brigham and Women’s Hospital to try to block a policy that requires employees to receive flu vaccines. The Brigham and Women’s policy requires that all workers be vaccinated annually, with exceptions for medical or religious reasons. In addition, similar to the VA rule, employees who opt out of flu immunization must wear face masks when working. The case was dismissed because the judge ruled the union didn’t have standing to bring the complaint, but the merits weren’t adjudicated.
Many other lawsuits against healthcare organizations have been filed around the country because of flu vaccination policies, including in Asheville, NC, Springfield, MA and Erie, PA. In addition, for unionized healthcare systems, including the VA, mandatory vaccination requirements often are an issue in collective bargaining negotiations.
The upshot tends to be relatively low vaccination rates for some types of personnel when not required. For example, an article last year in the Morbidity & Mortality Weekly Report noted that the vast majority of physicians got a flu shot before the 2015-16 influenza season but the rates were much lower among assistants and aides. Coverage generally was highest among physicians, nurse practitioners/physician assistants, nurses, pharmacists and healthcare personnel working in hospital settings.2
Specifically, based on an opt-in Internet panel survey conducted by the national Centers for Disease Control and Prevention (CDC), vaccinations continued to be higher among healthcare personnel working in hospitals (91.2%) and lower among healthcare personnel working in ambulatory (79.8%) and long-term care settings (69.2%).
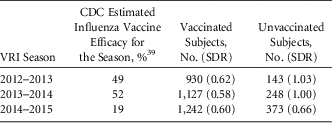
Coverage remained highest among physicians (95.6%) and lowest among assistants and aides (64.1%), and highest overall among healthcare personnel who were required by their employer to be vaccinated (96.5%), the CDC reported.
While publicly available statistics on overall HCP flu immunization are outdated at the VA, a recent survey by the state of Utah gives a snapshot; while the overall HCP influenza vaccination rate was 95.2%, it was 66% for the VA Health System located there.
“Immunization is a primary influenza prevention strategy. Since 1984, the Advisory Committee for Immunization Practices (ACIP) has recommended annual influenza vaccination for healthcare personnel (HCP),” authors of the recent study pointed out.
Background information in the article stated that, in 2008, the Centers for Disease Control and Prevention (CDC) estimated that only 49% of HCP in the United States had received the influenza vaccine by the 2015-2016 season, that number has increased to 79%, with vaccination rates highest, more than 95%, where employers required its use.
On the other hand, the study emphasized that “the secondary benefits and rationale for mandatory HCP vaccination policies remain controversial.” Past studies have disagreed on whether influenza vaccination of HCP has effect on absenteeism.
1Frederick J, Brown AC, Cummings DA, Gaydos CA, et. Al. Protecting Healthcare Personnel in Outpatient Settings: The Influence of Mandatory Versus Nonmandatory Influenza Vaccination Policies on Workplace Absenteeism During Multiple Respiratory Virus Seasons. Infect Control Hosp Epidemiol. 2018 Apr;39(4):452-461. doi: 10.1017/ice.2018.9. Epub 2018 Mar 8. PubMed PMID: 29514719.
2Black CL, Yue X, Ball SW, Donahue SM, et. Al. Influenza Vaccination Coverage Among Health Care Personnel – United States, 2015-16 Influenza Season. MMWR Morb Mortal Wkly Rep. 2016 Sep 30;65(38):1026-31. doi: 10.15585/mmwr.mm6538a2. PubMed PMID: 27684642.
