FORT MEADE, MD — With pharmacists from across the DoD and VA clamoring for spots in the Clinical Pharmacy Course at Army Medical Department Center and School (AMEDDCS) in Fort Sam Houston, TX, organizers offered back-to-back programs this spring, with another scheduled for August.
“We had so many applicants in February, that we did a quick repeat in March,” said course director Jennifer Evans, PharmD, clinical pharmacy coordinator at Fort George G. Meade, MD. The additional class allowed most of the 70 applicants for the February session to receive training over the two months. The August training will be the first time the course has offered three sessions in one year.
The expansion reflects the burgeoning demand. While the program began as an Army-branded course, growing participation from the Navy and Air Force, as well as the VA, has put the course on track to become a triservice program under the Defense Health Agency, Evans told U.S. Medicine.
The program started in February 2016 when Leslie Walthall, PharmD, and John Spain, PharmD, the former Army Office of the Surgeon General pharmacy consultant, recognized the need to quickly train clinical pharmacists as the Army ramped up its hiring to manage polypharmacy issues. In addition, as some clinical pharmacists are the only ones in their health clinics, the course was designed to “give people coming new to our brand of clinical pharmacy the tools to succeed and drive clinical pharmacy forward,” Evans said.
In addition to four sessions held in Texas, the course has trained pharmacists stationed overseas in sessions offered in Europe and Asia. Many participants in the course receive funding through the Medical Education and Training Campus (METC), which has provided “huge support for continuing pharmacy education,” Evans said. Pharmacists and technicians not eligible for METC funding have received local support to attend the program. Students may receive up to 34 hours of Accreditation Council of Pharmacy Education Continuing Pharmacy Education (CPE) credits for the course.
Pharmacists see significant value in the course beyond meeting CPE requirements. One said, “This was the best course I have ever taken. I will use more of the information than I thought possible.” Another commented, “So many topics directly addressed how an Army clinical pharmacist can successfully fulfill their responsibilities.” One pharmacist cut to the heart of challenge many clinical pharmacists face: “This boot camp course was vital to help me to continue to validate clinical pharmacy at my location!”
Each session trains about 25 pharmacists and five pharmacy technicians. During the “draining, intense week,” Evans said participants learn practical skills to increase efficiency, improve management skills and document the value of clinical pharmacy and gain a greater understanding of the role of clinical pharmacists in force readiness and the medical home. Pharmacy technicians have a few classes dedicated specifically to their needs and issues, including helping to identify at-risk patients, pharmacy communications, appointment scheduling and supporting clinical pharmacy services.
Many of the classes focus on training in key topics such as battlefield acupuncture, diabetes foot examinations, medication reconciliation, polypharmacy, opioid reduction strategies, smoking cessation strategies, post-traumatic stress disorder pharmacotherapy and physical examinations.
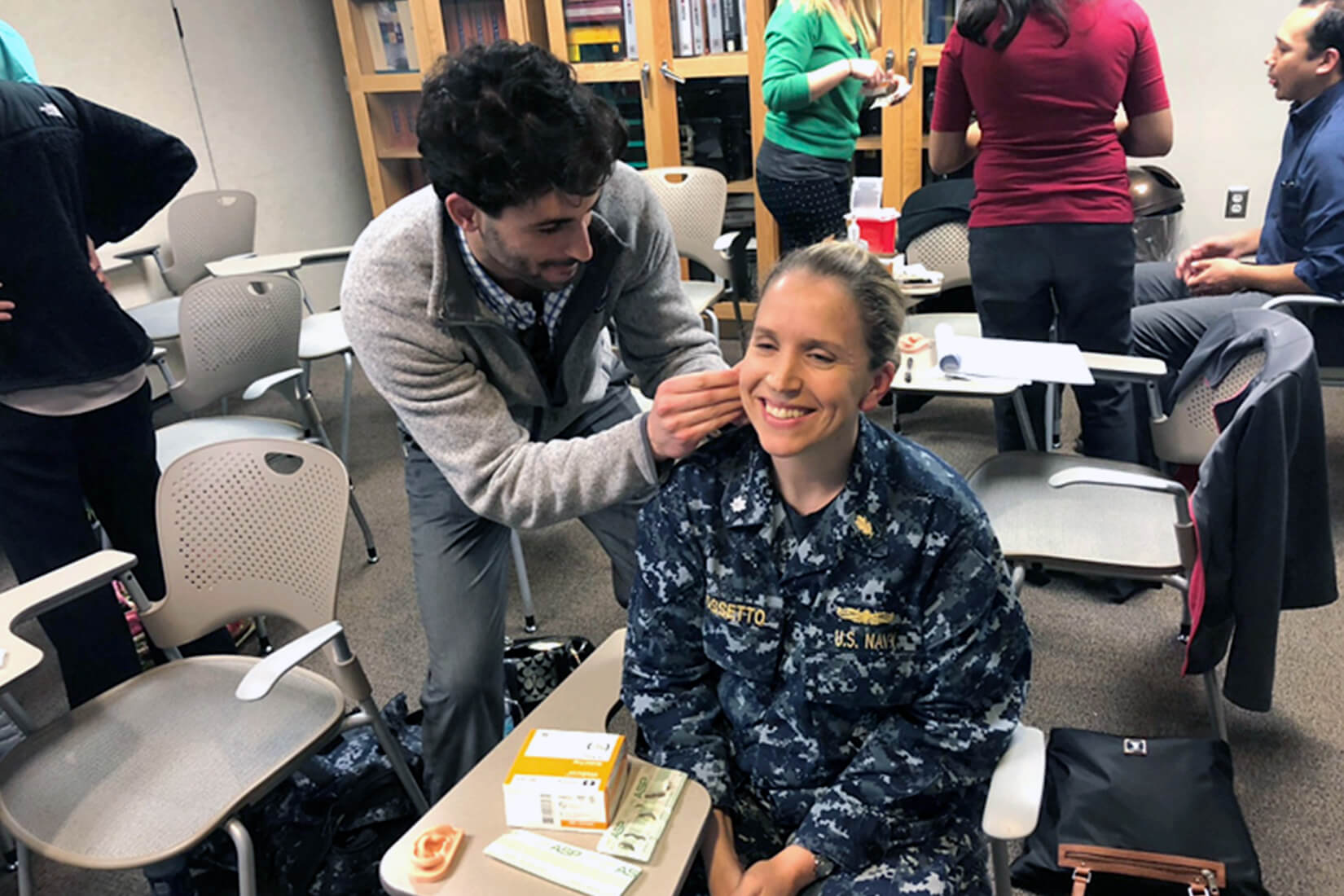
Acupuncture has been “a really unexpected but booming business for pharmacists,” Evans said. “With the focus on polypharmacy and trying to reduce opioid use, acupuncture is a handy back pocket skill to utilize for non-drug treatment in patients who have been using a lot of pain medication.” The acupuncture training uses a technique developed by Richard Niemtzow, MD, PhD, MPH, and managed by the U.S. Air Force Acupuncture Center. Pharmacists insert a fine needle into five points on each ear to reduce pain. Evans noted that acupuncture provides a safe alternative for high-risk patients and gives pharmacists an opportunity to educate patients while treating them.
Diabetic foot examination techniques were added to the course after the Army established diabetes care Healthcare Effectiveness Data and Information Set (HEDIS) metrics to the pharmacy service line. Pharmacists work the exam in when they see patients with diabetes for medication consults or other reasons. Pharmacists receive training on use of a monofilament, tuning fork and reflex hammer for the exam as well as how to recognize signs of developing diabetic damage.
“We now include about four hours of hands-on training with the CarePoint database, so clinical pharmacists and clinical pharmacy technicians can use it to help medical teams identify high-risk patients,” Evans said. Those could include diabetics who need medication adjustments or an annual foot exam, patients with polypharmacy concerns or use of high dose opioids.
The greatest impact of the course has been seen in standardizing the value of clinical pharmacy services and efforts by clinical pharmacists to contribute to force readiness, Evans added. Increasing familiarity with the full functionality of the AsUType, CarePoint and AHLTA systems contributes to those goals by significantly improving efficiency and freeing time for more patient interaction. “People have really valued that in our standardization,” Evans noted.
For each participant, the organizers look at key metrics three months before the course and three months after the course. Based on those evaluations, the course provides significant value to the Army. “We’ve seen consistent improvement in time in patient care and HEDIS metrics,” she said.
Evans attributed the program’s popularity and positive outcomes to the participants’ commitment. “All the students that attend are charged with a mission to implement what they have learned, to continue to prioritize clinical pharmacy contributions to readiness. The course has really been a success from all the enthusiasm attendees bring to the course, ready to learn and then what they take back to their clinics to implement change.”
