By Brenda L. Mooney
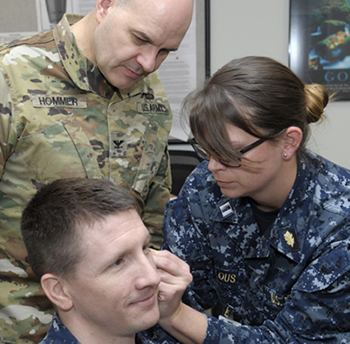
Army Col. Dean Hommer (left), a visiting instructor from Brooke Army Medical Center at Fort Sam Houston, TX, observes as Navy nurse Lt. Rachael Wheelous (right) practices the battlefield acupuncture technique on Navy nurse Lt. Brent Pavell (center) during training at Naval Health Clinic Corpus Christi, TX. A survey found that the MHS is taking a leadership role in using complementary and alternative medical procedures. Navy photo by William Love
SANTA MONICA, CA—The military health system has taken a leading position with the availability and usage of complementary and alternative medicine (CAM)W.
A report published in the Journal of Alternative and Complementary Medicine notes that most MTFs offer at least one type of CAM, and an estimated 76,000 military patients receive integrative health services each month.1
The study team included RAND Corp. researchers in Santa Monica and Pittsburgh, as well as participation from the San Antonio Military Medical Center at Fort Sam Houston, TX.
Included in the article are detailed data on the specific types of CAM offered by the MHS, the conditions for which they are used and their levels of use.
“Surveys of military personnel indicate substantial use of complementary and alternative medicine (CAM) that possibly exceeds use in the general U.S. population,” study authors noted. “Although military treatment facilities (MTFs) are known to offer CAM, surveys do not indicate where servicemembers receive this care.”
With the data, they added, MHS policymakers can “better support their population’s healthcare needs.”
Responses were received from 133 of the 142 MTFs in the MHS, 94%. Results indicated that, of these, 110 (83%) offer at least one type of CAM and five more plan to offer CAM services in the future.
Most likely to offer CAM services and more than 10 different types were larger MTFs with more than 25,000 beneficiaries enrolled, according to the survey. Results indicated the following:
- Three-fourths of MTFs offering CAM provide stress management/relaxation therapy,
- Two-thirds provide acupuncture, and
- At least half provide progressive muscle relaxation, guided imagery, chiropractic and mindfulness meditation.
“MTFs most commonly report CAM use for pain and mental health conditions,” the researchers found. “Acupuncture and chiropractic are most commonly used for pain, and stress management/relaxation therapy and mind-body medicine combinations are most often used for mental health-related conditions. We estimate 76,000 CAM patient encounters per month across the MHS.”

Soldiers with the 2nd Brigade Combat Team, 101st Airborne Division (Air Assault) participate in yoga during one of the weekly classes offered by Joined Forces Yoga at Fort Campbell, KY. Photo by Sgt. Sierra A. Fown, 2nd Brigade Combat Team, 101st Airborne Division (Air Assault) Public Affairs
- Writing in a white paper for the RAND Corp. last year, the same authors said CAM services required 1,750 full-time equivalents of staff and contractor time annually, a minimum labor investment of $112.7 million per year, adding, “Patient visits for CAM make up a small but nontrivial portion of total outpatient MTF visits.”2
Study authors also pointed out that the MHS is incorporating the use of integrated health services into its clinical practice guidelines.
- “Military health facilities report that they are using these treatments because they’ve found that they work for specific conditions,” explained lead author Patricia Herman, ND, PhD, Senior Behavioral Scientist at RAND Corp. and an associate editor of JACM. “They are one more tool in the tool kit for dealing with issues like chronic pain, and they can offer an alternative to opioid drugs.”The white paper noted that the most common reasons for MTFs to not offer CAM is the difficulty in finding providers. The authors also point out, “In general, our study’s findings about CAM in MTFs are quite similar to results of the VA’s CAM survey conducted in 2011, such as percentage of facilities offering CAM and the number of CAM types offered, among other findings.”
In terms of improving delivery, the researchers suggested a lack of consistency in the criteria used for credentialing and privileging CAM providers and called for better documentation and coding of the use of CAM services.
In the white paper, they made the following recommendations:
- Standardize coding for CAM services to allow for consistent tracking of the types of CAM services being offered, their provider types and the conditions for which they are used and will allow better manpower management, a better record for physicians about the other treatments that patients are receiving, and easier data collection for future comparison studies.
- Conduct a medical record review at a small number of MTFs to validate survey findings and MHS utilization data to validate the data collected through the CAM survey.
- Address CAM in clinical guidelines for conditions for which it is frequently used, especially since most MTFs cited scientific evidence as a reason to offer their CAM therapies.
- Standardize credentialing and privileging for providers of CAM services to ensure that the providers are properly and consistently trained.
- Target future research toward the CAM services with reported success to help other MTFs add the services.
The editor of JACM , John Weeks, suggested, meanwhile, that the military’s role in making CAM more acceptable is somewhat surprising.
“An irony of the military’s uptake of practices that 40 years ago were associated with the counterculture is that we may one day soon view this accrued experience as a source of soft technology transfer from the military to better integrate these pain and mental health practices in civilian healthcare,” Weeks noted.
- Herman PM, Sorbero ME, Sims-Columbia AC. Complementary and Alternative Medicine Services in the Military Health System. J Altern Complement Med. 2017 Nov;23(11):837-843. doi: 10.1089/acm.2017.0236. Epub 2017 Oct 17. PubMed PMID: 29039681.
- Herman, PM, Sorbero, ME, Sims-Columbia. SC, Complementary and Alternative Medicine in the Military Health System. Santa Monica, CA: RAND Corporation, 2017.

