By Annette M. Boyle
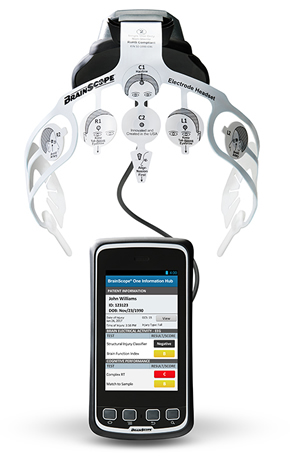
The portable and durable BrainScope assesses electrical activity in the brain to detect internal bleeding prior to a CT scan and could be used in a number of military scenarios, according to military researchers. Photo from the manufacturer.
WASHINGTON—Neuroscientists are tackling some of the challenges to brain health predominantly experienced by servicemembers – and that has important implications for the broader population.
Two recent studies address the chronic multisymptom disease known as Gulf War Illness (GWI). Nearly 32% of veterans of the 1990-1991 Gulf War experience a variable combination of functional medical issues such as muscular fatigue, chronic pain, vision disturbances and gastrointestinal disorders, as well as neurological concerns including impaired memory, attention and mood. “These associations emphasize the interconnectedness of the brain and body,” noted the Institute of Medicine (now the Health and Medicine Division) in its most recent report on the condition.
Recent research indicates that sarin gas, which was used widely as a nerve agent during the conflict, contributes to development of GWI. While high doses of sarin are fatal, research presented at the annual meeting of the Society for Neuroscience demonstrated that low doses of sarin, combined with high levels of stress, suppress dopamine and destabilize microtubules that provide support and facilitate transport in neurons. Impaired dopamine release is associated with a number of neurodegenerative diseases.
The researchers also identified a way to reverse the effects of sarin. In tests with rats, the molecule tubacin restored the proper structure of the microtubules. Now, the researchers are confirming their findings with neurons derived from stem cells from Gulf War veterans.
This “will more closely mimic the disease state and provide a more detailed understanding of the effects of stress in Gulf War Illness and thereby help us to test medicines that may improve the health of veterans,” explained lead author Ankita Patil, MS, of Drexel University College of Medicine.
Other research presented at the conference documented extensive communication abnormalities in neurological networks of veterans with GWI. The team of researchers from Atlanta and Houston used functional magnetic resonance imaging (fMRI) to compare communication patterns in various brain regions in 22 veterans with GWI to those of 30 age-matched veterans without the disease.
They found that the brains of affected veterans exhibited neural communication deficits that affected visual processing, mood regulation, motor coordination, sensory processing and language. The patients also had heightened communication in sectors that corresponded to pain perception during rest. “The results from this study provide strong evidence of neuropathology in GWI patients from exposures to neurotoxic agents,” pointed out lead author Kaundinya Gopinath, PhD, of Emory University. The next step, she said, was to “establish brain mechanisms underlying GWI, which in turn can lead to development of treatments.”
TBI Research
Recent research has also made significant strides in improving diagnosis of and treatment for the signature injury of recent conflicts—traumatic brain injury (TBI). One new test helps providers assess TBI more accurately by determining whether a patient’s eyes are tracking properly, explained Tracie Lattimore, MSN, NP, chief, Army Traumatic Brain Injury Program. Up to 60% of veterans with TBI experience oculomotor dysfunction.
Two new devices will also help providers evaluate patients with potential head trauma. The portable and durable BrainScope assesses electrical activity in the brain to detect internal bleeding prior to a CT scan and could be used in a number of military scenarios, while the InfraScan employs near-infrared spectroscopy to identify potential bleeding in the brain.
Research on college athletes and others has also contributed to TBI prevention and care. “There has been a marked recognition of TBI as a public health problem that needs expertise, resources and research. The military has been able to partner with our federal and private sector colleagues to advance the science still further,” Louis French, PhD, deputy director, Walter Reed National Military Medical Center’s National Intrepid Center of Excellence, told U.S. Medicine.
A study by the National Collegiate Athletic Association and the DoD Grand Alliance, for example, revealed two significant factors in concussions. First, it showed that many athletes who experienced a TBI had suffered one or more sub-concussive hits in the preceding hours or days, indicating that the effect of hits build on one another, according to Lattimore.
The second finding came from a comparison of players who experienced a concussion in 2002 vs. those who had one in the last few years. In the earlier period, players returned to the game within a few days of a concussion—and then experienced a more severe concussion 5.2 days later, on average, she said.
Today, players remain on the bench until they exhibit no symptoms of concussion, usually 12 to 14 days after the injury. Second concussions do not occur until 72 days later and are much less serious than the second concussion experienced by players in 2002.
“This study validates the DoD’s hallmark policy for concussion management in deployed settings, which beginning in 2010 removed soldiers who sustained a concussion from duty until symptom-free,” Lattimore said.
Removing a soldier from battle or training to fully recover optimizes capability on return, while reducing frequency and severity of additional injuries, she added. “That message needs to be communicated, not just to medical personnel, but to every Army leader.”

