NASLD Is A Leading Risk Factor for Hepatocellular Carcinoma
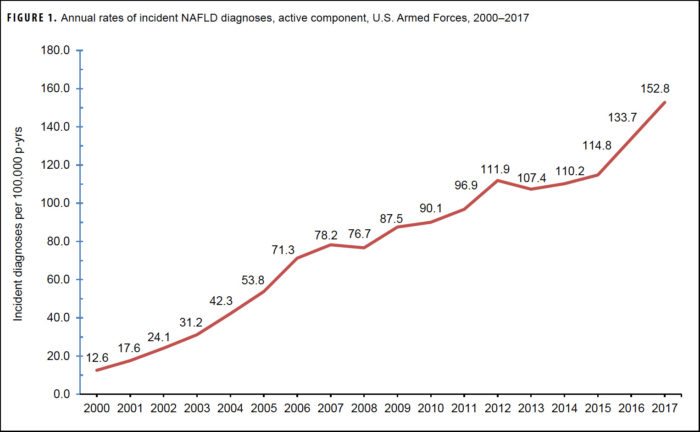
Over the last 17 years, the incidence of nonalcoholic fatty liver disease among active-duty U.S. military servicemembers leapt from 12.6 cases per 100,000 person-years to 152.8. In the short term, military personnel with impaired liver function are barred from service. What is especially disturbing is in the longer term, as recent research has demonstrated a strong link between NASLD and risk of hepatocellular carcinoma.
HOUSTON—In the United States, the incidence rate of hepatocellular carcinoma is increasing, although the pace may have somewhat slowed since 2010. What might be most troubling for the military medical system, however, are recent epidemiological changes in major risk factors for the most common liver cancer.
A report last month in Current Gastroenterology Reports pointed out that those risk factors include increasing hepatitis C virus post-sustained virologic response, suppressed hepatitis B virus on nucleoside analogues and alcoholic and nonalcoholic fatty liver disease.1
“Non-alcoholic fatty liver disease has the greatest proportion of the burden of the main risk factors for HCC in the USA, followed by alcoholic liver disease, and hepatitis C virus and hepatitis B virus infections,” wrote the authors from the Michael DeBakey VAMC and Baylor College of Medicine, both in Houston.
That article followed the revelation in the Defense Health Agency’s Medical Surveillance Monthly Report that, during 2000-2017, a total of 19,069 active component servicemembers received incident diagnoses of nonalcoholic fatty liver disease, for a crude overall incidence rate of 77.7 cases per 100,000 person-years.2
The increased incidence of NAFLD was rapid, according to the report, jumping 12.6 to 152.8 cases per 100,000 person-years between 2000 and 2017.
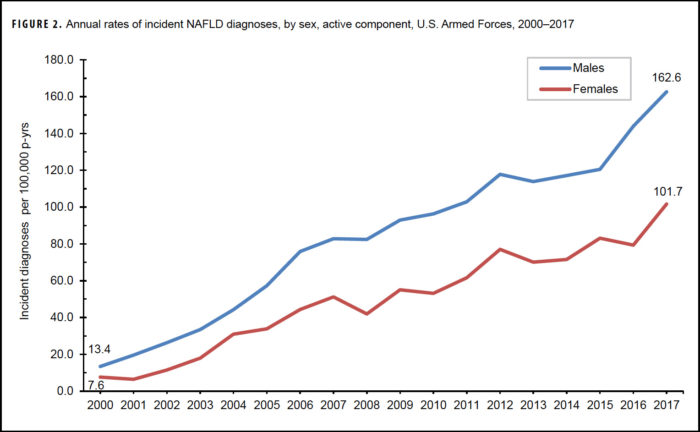
The article stated that the overall rate of incident NAFLD diagnoses among males was more than 1.5 times the rate among females and that overall incidence rates increased with advancing age and were highest among military personnel 50 years or older.
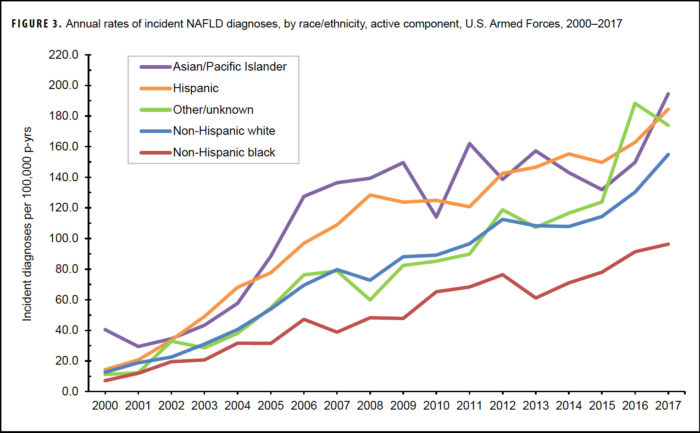
The highest overall incidence was in Asian/Pacific Islander and Hispanic servicemembers, compared to those in other race/ethnicity groups, the researchers said, adding that the lowest overall incidence by race/ethnicity was observed among non-Hispanic black service members.
Perhaps most alarming was that crude annual incidence rates of NAFLD diagnoses increased 12-fold between 2000 and 2017. “During this period, annual rates of incident NAFLD diagnoses increased in both sexes and in all age groups. Increases in annual rates were seen over time in all race/ethnicity groups and in all services,” the researchers explained. “More than two-thirds of incident NAFLD cases had one or more diagnosed metabolic comorbidities, with dyslipidemia affecting the greatest percentage of cases, followed by obesity/overweight and hypertension.”
In fact, they reported that the percentage of NAFLD cases with two or more metabolic comorbidities increased 36.0% during the 18-year surveillance period from 22.2% in 2001 to 30.2% in 2017.
In the short term, readiness is affected. Servicemembers with severe NAFLD resulting in impaired liver function are unable to perform their military duties and are disqualified from service. In the longer term, however, the repercussions could be extremely serious and have a significant effect on the DHA and VA.
NAFLD, HCC Link
A study also involving Houston VAMC and Baylor researchers suggested that NAFLD is a very common disease and that, with the incidence of liver cancer rising across the country, little has been understood about the link between NAFLD and HCC.3
The large, retrospective study of patients with and without NAFLD was reported in the journal Gastroenterology. Participants were a diverse cohort of patients—about 300,000 with and about 300,000 without NAFLD—from 130 facilities in the VHA, who were followed for about 11 years.
Of the patients with NAFLD, 490 developed HCC, leading the study team to conclude that the risk of developing HCC was much higher in patients with than those without NAFLD.
“Most importantly, we found that the risk for hepatocellular carcinoma is significantly higher in those patients with NAFLD, and this is the first large, diverse cohort study to quantify that risk,” said first author Fasiha Kanwal, MD, of the VA’s Health Services Research and Development Center for Innovations.
“Although, the absolute risk for HCC in NAFLD patients is low, it is still higher than the accepted threshold for HCC screening in the subset with established cirrhosis of the liver,” Kanwal said.
Patients with NAFLD who had developed cirrhosis of the liver had the highest incidence annually of HCC, according to the researchers, who also documented that the risk for HCC increased with age and that older Hispanics with cirrhosis were at the highest risk for HCC.
“This study provides valuable and robust information about who among the millions of people with NAFLD are at risk of developing HCC. The information is a significant step forward in our understanding of the disease, and will be of use to researchers, clinicians and patients,” explained senior author Hashem El-Serag, MD.
As for the study finding increasing rates in the military, an editorial comment suggested several possible explanations, noting, “As in the general population, the increase in NAFLD incidence among active component service members may be due, at least in part, to an increase in median BMI and increasing rates of clinical overweight.” The article also raised the possibility that an increasing trend in abdominal ultrasound testing seen in the MHS during 2000-2015 could be a contributor to the increasing trend in NAFLD diagnosis rates.
The greatest likelihood, however, is that the military is following trends already recognized in the civilian population, according to the authors.
“More than two-thirds of incident NAFLD cases had one or more diagnosed metabolic comorbidities, with dyslipidemia affecting the greatest percentage of cases, followed by obesity/overweight and hypertension,” they emphasized. “Moreover, the percentage of NAFLD cases with two or more metabolic comorbidities increased 36.0% during the 18-year surveillance period from 22.2% in 2001 to 30.2% in 2017. A similar trend in metabolic comorbidities over time has been noted in at least one large administrative data-based U.S. study; however, the magnitude of the increase over time seen in the general population was greater (21% to 53%). This difference in magnitude is likely due to differences between the populations in terms of age and overall health status. Regardless of this difference, the slight trend of increasing dysmetabolic burden over time observed among incident NAFLD cases in the current study suggests that the clinical profile of those with NAFLD is becoming more complex, because of the presence of more metabolic comorbidities near the time of NAFLD diagnosis.”
A recent meta-analysis in the journal Transplantation raised the question of whether patients with NAFLD should be regularly screened for HCC. International authors, including U.S. researchers from the University of California San Francisco and Houston Methodist Hospital, noted that, while patients with nonalcoholic fatty liver disease are at risk of developing hepatocellular carcinoma, the magnitude of the association still needs to be determined to define the need for a specific surveillance strategy.4
That conclusion was based on a search that identified 328 abstracts and ultimately included 25 studies.
The review pointed out that, considering only studies strictly including patients with or without cirrhosis, the reported incidence of HCC in NAFLD patients with cirrhosis was between 6.7 and 15% at five to 10 years, and the incidence in NAFLD patients without cirrhosis was 2.7% at 10 years and 23 per 100,000 person-years.
“Hepatocellular carcinoma screening in NAFLD patients with cirrhosis is mandatory,” the authors wrote. “However, the currently observed low (and insufficiently documented) incidence of HCC in NAFLD patients without cirrhosis does not justify a systematic surveillance. Research efforts should focus on developing a score, which could aid the clinician in identifying NAFLD patients without cirrhosis who are at higher risk of developing HCC.”
1 Kim HS, El-Serag HB. The Epidemiology of Hepatocellular Carcinoma in the USA. Curr Gastroenterol Rep. 2019 Apr 11;21(4):17. doi: 10.1007/s11894-019-0681-x. Review. PubMed PMID: 30976932.
2 Williams VF, Taubman SB, Stahlman S. Non-alcoholic fatty liver disease NAFLD), active component, U.S. Armed Forces, 2000-2017. MSMR. 2019 Jan;26(1):2-11. PubMed PMID: 30681879.
3 Kanwal F, Kramer JR, Mapakshi S, Natarajan Y, Chayanupatkul M, Richardson PA, Li L, Desiderio R, Thrift AP, Asch SM, Chu J, El-Serag HB. Risk of Hepatocellular Cancer in Patients With Non-Alcoholic Fatty Liver Disease. Gastroenterology. 2 Dec;155(6):1828-1837.e2.
4 Reig M, Gambato M, Man NK, Roberts JP, Victor D, Orci LA, Toso C. Should Patients With NAFLD/NASH Be Surveyed for HCC? Transplantation. 2019 Jan;103(1):39-44. doi: 10.1097/TP.0000000000002361. PubMed PMID: 30080818.
