Because of their cardiovascular protective effects, SGLT2 inhibitors have been a game-changer in Type 2 diabetes treatment. That is especially the case, now that the FDA has approved a new indication for canagliflozin to reduce the risk of major adverse cardiovascular events in adults with Type 2 diabetes who have established cardiovascular disease. Importance of the drug class could grow in the future, as ongoing studies look at the use of SGLT2 inhibitors to treat heart failure and other CV conditions.
MINNEAPOLIS—It’s common knowledge that the presence of both diabetes and heart disease in a patient can have a cumulative effect, with one disease negatively impacting the treatment options of the other.
Now, however, researchers are finding that the axiom also works in reverse. Treating Type 2 diabetes can improve that patient’s cardiovascular health. One of those treatments—sodium-glucose cotransporter 2 (SGLT2) inhibitor, a class of glucose-lowering drug—has been found to accomplish both simultaneously, improving cardiovascular outcomes while reducing glucose levels. Researchers are examining whether it might even improve outcomes in patients already suffering from heart failure.
“I’ve always been interested in the interplay between diabetes and heart disease,” explained Orly Vardeny, PharmD, an investigator at VA’s Center for Care Delivery and Outcomes Research. “We know patients with diabetes are at a much higher risk for developing heart disease. And when they do have heart disease, their risk for complications or bad outcomes are greater. It’s a synergistic effect having both.”
Vardeny has been studying the effects of SGLT2 inhibitors for years in patients with heart disease, tracking its effects on cardiovascular outcomes compared to a placebo. Previous glucose-lowering drugs were found to worsen heart failure. So, in 2008, the FDA mandated drug companies working on new glucose lowering therapies take into account the drug’s safety in regard to cardiovascular events. This extra layer of safety revealed something unexpected. Not only did SGLT2 not show any harmful effects on cardiovascular health, it seemed to prevent new heart failure and new heart failure hospitalizations.
“The first data came in 2015 from the EMPA-REG trial, which looked at the effects of the SGLT2 inhibitor empagliflozin,” Vardeny explained. “Researchers discovered that the drug reduced deaths from cardiac reasons, as well as hospitalizations from heart failure. A couple of other studies came out in succession using other SGLT2 inhibitors that showed the same thing.”
In December 2016, the Food and Drug Administration approved a new indication for empagliflozin, Jardiance for the reduction of heart-related deaths in people with Type 2 diabetes and established heart disease. Last fall, the FDA approved canagliflozin, marketed as Invokana, to reduce the risk of major adverse cardiovascular events in adults with Type 2 diabetes who have established cardiovascular disease.
How exactly SGLT2 inhibitors achieve this protective cardiovascular effect isn’t entirely understood, however, Vardeny pointed out.
“That’s the $50,000 question,” she said. “We think we know some of the mechanisms but not all of them. The most obvious is through the inhibitor’s actions in the kidney to prevent the reabsorption of sodium. Your body gets rid of water. You have less edema. Excess fluid is the hallmark of heart disease. But there are a lot of other potential mechanisms. Some may be through direct actions on this sodium hydrogen exchanger in the heart and heart cells and kidney cells that may be protective.”
One study, the EMPA-HEART trial, found patients taking empagliflozin had reverse remodeling of their hearts. “Patients who had enlarged hearts, which happens over time with heart disease—that process reversed itself,” Vardeny explained. “We think it’s a direct beneficial effect on how the heart remodels in response to stress. There are a lot of mechanistic studies going on right now trying to figure this out.”
Heart Failure Treatment?
The protective effect of the inhibitors is so significant, that researchers began to wonder whether it would have a similar effect on patients already suffering from heart failure. At least four trials are currently underway looking at SGLT2 inhibitor’s effects on patients with either systolic or diastolic heart failure. Vardeny is the lead investigator on the DELIVER trial, which is evaluating the SGLT2 inhibitor dapagliflozin’s effects on patients with systolic heart failure.
“We’re looking to see whether it improves cardiovascular outcomes compared to placebo. These are patients who may or may not have diabetes. That’s a hot topic right now in terms of heart failure—figuring out whether this class of glucose-lowering therapy improves outcomes in people with heart failure even if they don’t have diabetes,” Vardeny explained. “We’ll know the results in November 2019.”
Currently, SGLT2 inhibitors are only approved in people with Type 2 diabetes. But both the American Diabetes Association and the European Association for the Study of Diabetes strongly recommend SGLT2 as a second line medication, after metformin, for patients with both diabetes and heart disease.
“The word is spreading that it has a cardioprotective effect and that it reduces heart failure,” Vardeny said. “But the question a lot of clinicians struggle with is where do they fit within the spectrum of the glucose-lowering therapies that are available right now. Partially because they’re more expensive. The struggle is that there’s always a lag time between major trials and uptake of therapies into clinical practice. And there’s a little bit of clinical inertia and hesitancy when it comes to new therapies.”
Part of that hesitancy in this particular case is that it’s asking cardiologists to step outside of their treatment comfort zone. “It’s a new area for cardiologists because they’re not used to prescribing glucose-lowering medications,” Vardeny explained. “Now they’re being brought into the loop to use these therapies, but they’re not someone who’s comfortable managing diabetes as a cardiologist. It’s going to take a team effort between an endocrinologist, primary care doctor, and cardiologist.”
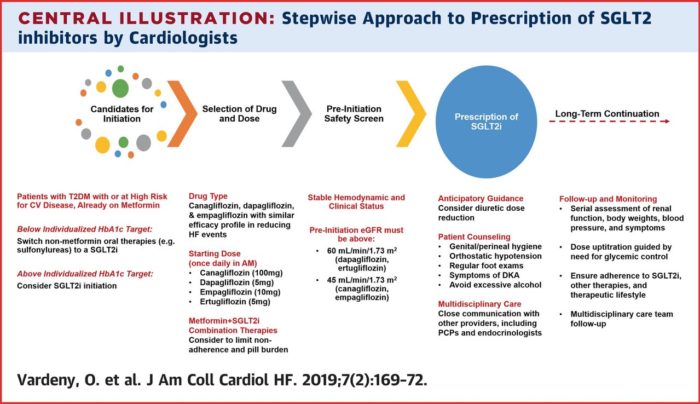
To help cardiologists make the leap, Vardeny and co-author Muthiah Vaduganathan, MD, of Brigham and Women’s Hospital Heart & Vascular Center and Harvard Medical School, both in Boston, wrote a “Practical Guide to Prescribing Sodium Glucose Cotransporter 2 Inhibitors for Cardiologists,” which leads cardiologists step-by-step from selecting patients who might benefit through long-term continuation of treatment.1
1 Vardeny O, Vaduganathan M. Practical Guide to Prescribing Sodium-Glucose Cotransporter 2 Inhibitors for Cardiologists. JACC Heart Fail. 2019 Feb;7(2):169-172. doi: 10.1016/j.jchf.2018.11.013. Review. PubMed PMID: 30704605.
