A new study looks at factors to improve survival rates in veterans with multiple sclerosis. VA’s efforts don’t stop there, however. The healthcare system has a multipronged effort to reduce disability and improve quality of life in MS patients, especially those with progressive and relapsing types of the disease.
OKLAHOMA CITY—This spring, the VA announced a partnership with the National Multiple Sclerosis Society to advance and improve the lives of the about 20,000 veterans treated for MS in the healthcare system.
“MS can be an overwhelming challenge for those who are fighting the disease and their loved ones who care for them,” said VA Secretary Robert Wilkie. “VA recognizes and values the strength of collaborations with our external partners, which can help increase access to care and lead to a more fulfilled quality of life.”
VA and the National MS Society seek to enhance health services, education and self-efficacy and promote whole health goals of veterans and their families by sharing certain resources and collaborating on policy, educational and research initiatives.
Veterans already have access to a national network of regional and support programs to improve their diagnosis and treatment with the 2003 establishment of VA’s MS Centers of Excellence.
Yet, some significant challenges remain in providing optimal care of MS patients, according to recent conference presentations. Two studies led by Meheroz H. Rabadi, MD, of the Oklahoma City VAMC were presented at the 2018 Consortium of Multiple Sclerosis Centers Annual Meeting in Nashville.
The first emphasized that the mortality rate in veterans with MS is 14% and is influenced by motor complaints at presentation, MS type and severity of the initial disease. Contributing factors included MS disease itself and MS-related complications, such as presence of infection and respiratory failure.
“Examining factors that increase risk of death in veterans with MS may help reduce MS-related mortality,” suggested Rabadi and his colleagues. Their goal was to determine the predictors of mortality in veterans with multiple sclerosis attending an out-patient clinic.
To do that, the study team conducted a retrospective review of electronic charts of 226 veterans with MS regularly followed in the Oklahoma City VAMC clinic from Jan. 1, 2000, to Dec. 31, 2014. Of the 226 participants included in the analysis; 17% were female and most were white. The mean age of MS diagnosis was 36, and the mean age of study entry was 49, with mean duration of MS of 21 years, and the mean duration of follow-up was 12 years.
Overall, 20% of participants had primary progressive MS, 24% had secondary progressive MS, 43% had relapsing-remitting MS, and 14% had another or unknown MS type.
Survivor Differences
When researchers compared those who survived vs. those who died over the 15-year period, significant differences were identified. Those who died were more likely to have:
- Progressive MS type,
- Worse initial motor presentation,
- Presence of motor weakness and ataxia on examination,
- Severity of the initial disease,
- Presence of neurogenic bladder, pressure ulcers, diabetes mellitus, and
- Lower body mass index
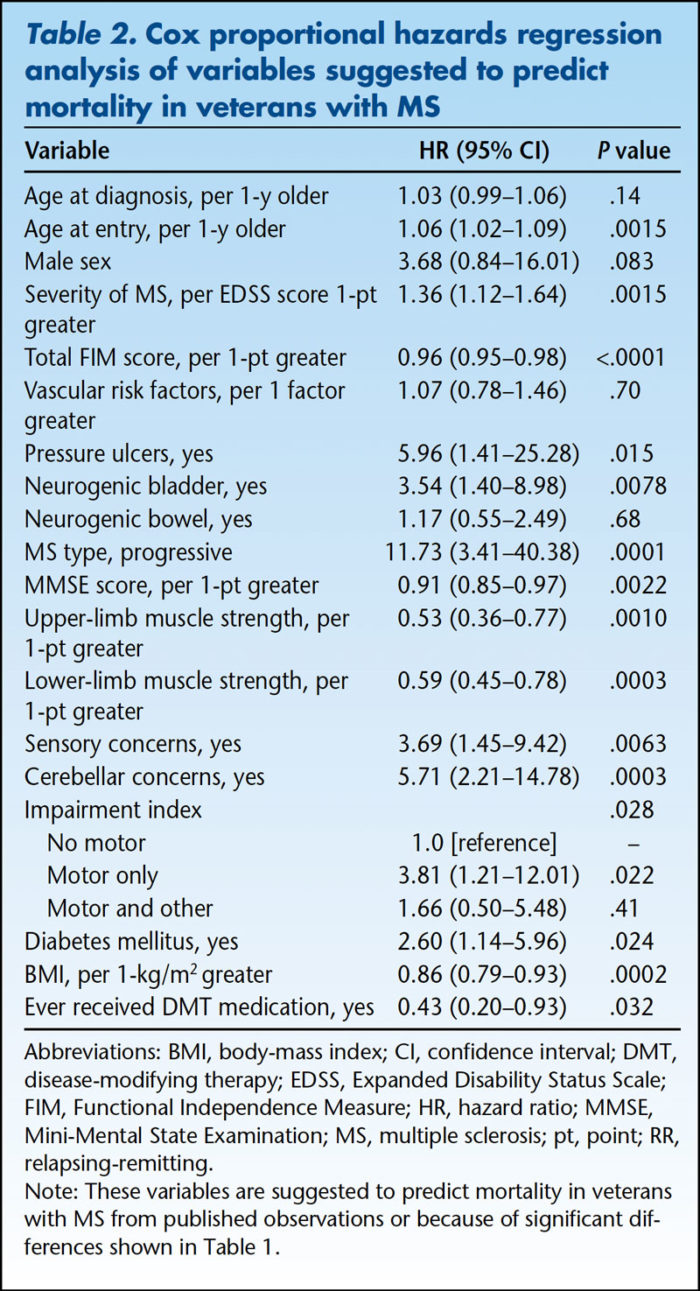
Researchers found that MS disease itself (57% of cases), infection (43%) and cancer and respiratory failure (18% each) were the likeliest causes of death. After analysis, MS type, severity of the initial disease and presence of pressure ulcers were identified as the main predictors of MS-related mortality.
Among patients who died during the follow-up period, 36% had primary progressive MS, compared with 17% of patients who were alive, while 42% of patients who died had secondary progressive MS, compared with 21% of those who were alive.
Other findings included:
- Patients who died had an average age of 56 at the beginning of the study, compared with an average age of 48 among those who were alive;
- BMI of those who died was an average of 23.7, compared with 28 among patients who were alive;
- More than one-third, 39%, of patients who died were never on a disease-modifying therapy, compared with 22% of patients who were alive;
- About one-third, 33%, of patients who died had diabetes mellitus, compared with 16% of those who were alive;
- 12% of patients who died had pressure ulcers, compared with 2% of patients who were alive; and
- 82% of patients who died had neurogenic bladder, compared with 53% of patients who were alive.
The study calculated that MS patients died prematurely with a standardized mortality rate 1.35 relative to the general (Oklahoman) population.
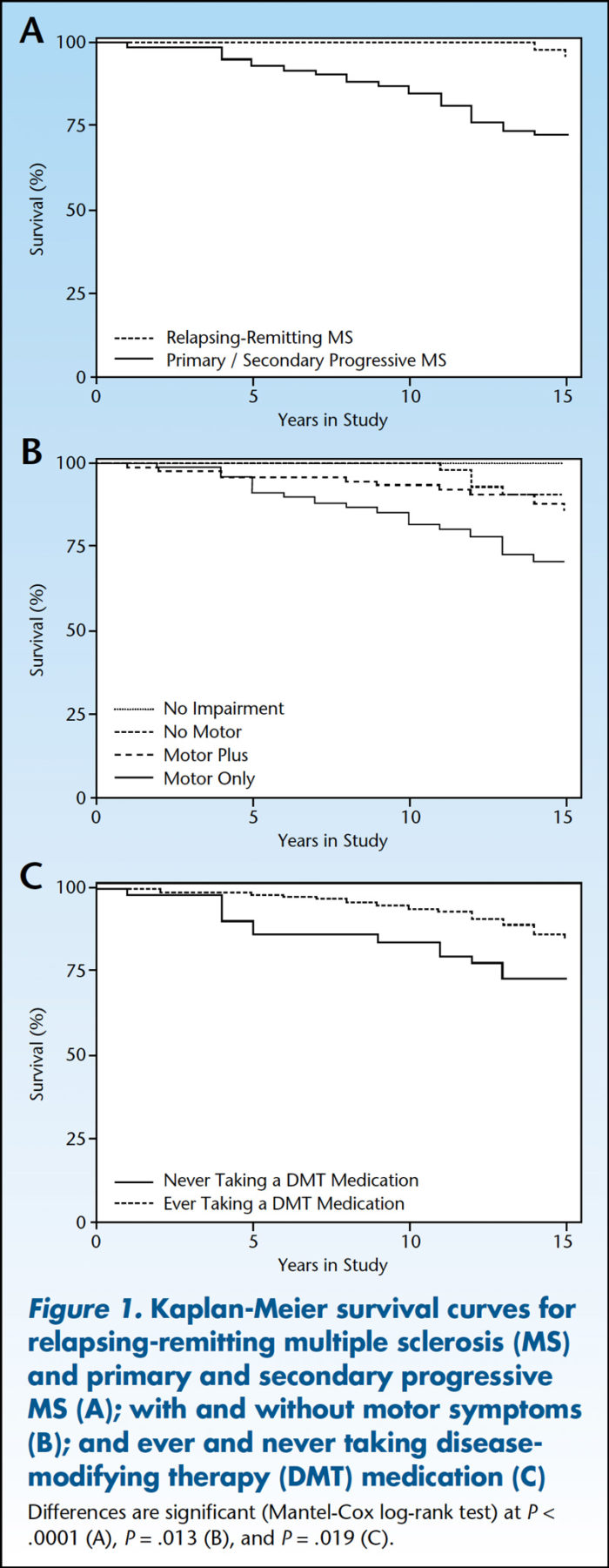
“Mortality rate in veterans with MS is 14%, and is influenced by motor complaints at presentation, MS type, and severity of the initial disease. MS disease itself and MS-related complications, such as presence of infection and respiratory failure were the contributing factors,” the study authors concluded.
An issue in long-term survival for MS patients was whether they also suffered chronic medical conditions, such as obesity, hypertension and arthritis, which are common in the general population and are responsible for functional limitations, increased hospitalization and increased mortality.
“Given that the risk of MS and the presence of CMCs increases with age, we wanted to study the impact of the presence of commonly encountered CMCs on long-term disability (activity limitation) in veterans already diagnosed with multiple sclerosis (MS),” Rabadi wrote.
The observational study sought to examine the effect of common chronic medical conditions on long-term disability (activity limitation) in veterans already diagnosed with MS.
To do that, the study retrospectively reviewed the electronic charts of 124 veterans with MS who had been regularly followed in the Oklahoma VAMC clinical for a decade or more. Using general linear model analysis, they examined whether MS-related severity as measured by the Expanded Disability Status Scale and the presence of CMCs affected long-term disability as measured by the total score on the Functional Independence Measure.
Results showed that commonly encountered CMCs were increased BMI (61%), hyperlipidemia (78%), hypertension (65%), current smokers (47%) and arthritis/arthralgia (24%). The findings suggested, however, that the number of CMCs was not predictive of final TFIM scores. Instead, of the variables examined, only initial EDSS score was predictive of final TFIM scores.
“The presence of CMCs did not affect the long-term disability in veterans diagnosed with MS, this was due mainly to CMCs being closely monitored and co-treated with other medical specialties,” Rabadi wrote.
Overall, based on the two studies, researchers advised that more attention be paid “to preventive strategies, such as yearly influenza immunization, aggressively treating MS-related complications and comorbidities, especially vascular risk factors.”
An article online from the VA’s Multiple Sclerosis Centers for Excellence website zeroed in on another factor identified in the mortality study—use of disease modifying therapies for MS.
DMT Importance
James Bowen, MD, of the VA Puget Sound Healthcare System in Seattle wrote that all VA patients with MS should discuss taking a DMT with their MS provider.
He pointed out that, when offered, most veterans choose to take them, adding, “Fortunately, we now have over a dozen different DMTs that slow the course of MS. These medications have all been proven to benefit MS patients in well-designed large studies. Based on the results of these studies, the MS Coalition states that starting DMT treatment should occur: ‘as soon as possible when a person has been diagnosed with relapsing or primary progressive MS, regardless of age.’ Because DMTs, like any medication, comes with risks, patients must decide for themselves, with the help of their doctors, whether they wish to start, stop, or continue use of these medications.”
Bowen emphasized that DMTs “are the only medications proven to slow the disease. After 20 years, 15-20% of untreated patients are in wheelchairs and another 50% need aids to walk. Use of these medications should improve these odds and lessen the disability that develops over time.”
The article offered several reasons why use of DMTs is lower than it should be in VA patients. Bowen said those include:
- Some patients believe they do not have enough attacks to warrant use of DMTs, a very conservative estimate is that patients have 10 silent attacks for every attack of which they are aware.
- Patients might not realize how serious thinking or memory loss can be and don’t make them a high priority.
- Some patients wait to see if they will become more disabled before using DMTs, although clinicians advise starting DMTs before more damage occurs.
Bowen wrote, “There is evidence that patients using DMTs early in the disease leads to better long-term responses than those treated later in the disease. This is true even after the first attack, called Clinically Isolated Syndrome, and several DMTs are FDA-approved in this early stage of disease.” He also adds that more DMTs are approved for patients who experience relapses than progressive forms without relapses, adding that only one DMT is approved for primary progressive MS.
And that has made a big difference, according to a review co-authored by Olaf Stüve, MD, PhD, of the VA North Texas Healthcare System in Dallas. Authors of the study published in Expert Opinion on Emerging Drugs noted last spring, “The recent approval of ocrelizumab is a major milestone forward in the therapy of PPMS. One reason for success of this drug is appropriate patient selection. The ultimate goal in PPMS therapy should be the reversal of disability, and the arrest of disease progression. Our current understanding of PPMS suggests that a combination of immune-modulatory, myelin-restorative, and neuro-regenerative therapies particularly early in the disease course would be a reasonable strategy. Finally, selection of appropriate patients, selection of appropriate outcomes and monitoring therapy is again crucial for success of therapeutic strategies.”
Roche, the manufacturer of the drug, marketed as Ocrevus, announced in the fall that new data showed early initiation of treatment reduces disability progression over five years in relapsing and primary progressive multiple sclerosis. In addition, patients with relapsing MS (RMS) treated sooner with Ocrevus had earlier reduction in disease activity and less disability progression vs. those who switched from interferon beta-1α.
At the same time, primary progressive MS (PPMS) patients treated with OCREVUS earlier had less disability and upper limb progression than those who switched from placebo
1 Rabadi, MH, Aston, CE. Predictors of Mortality in Veterans with Multiple Sclerosis in an out-Patient Clinic Setting. Paper presented at 2018 Consortium of Multiple Sclerosis Centers Annual Meeting. May 31, 2018. Nashville, TN
2 Rabadi, MH, Effect of Chronic Medical Conditions in Veterans with Multiple Sclerosis on Long-Term Disability. Paper presented at 2018 Consortium of Multiple Sclerosis Centers Annual Meeting. May 31, 2018. Nashville, TN
3 Ram Narendra Narayan, Thomas Forsthuber & Olaf Stüve (2018) Emerging drugs for primary progressive multiple sclerosis, Expert Opinion on Emerging Drugs, 23:2, 97-110, DOI: 10.1080/14728214.2018.1463370
