Military Medical Experts Educate Clinicians About Respiratory Support
One of the many challenges with treating COVID-19 is that acute respiratory distress syndrome associated with the infection is so different from what intensivists usually see. Another is that the influx of patients means that a lot of non-specialist physicians have been called on to care for these patients. In response, the Uniformed Service University of Health Sciences has created educational video series which provides critical information on ventilator usage and novel modes, such as airway pressure release ventilation, which allows for spontaneous breathing and has potential lung-protective benefits.
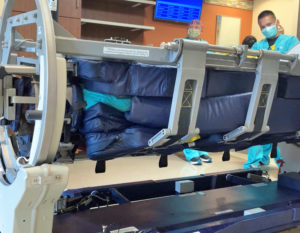
Col. Karin Nicholson is positioned inside the Carl R. Darnall Army Medical Center’s new rotating bed during an intensive care unit staff training session. Prone positioning therapy is one of the newest techniques being used in the intensive care unit improve outcomes for patients with acute respiratory distress syndrome (ARDS). Army photo by Mikaela Cade
BETHESDA, MD — The Uniformed Service University of Health Sciences has come to the rescue of non-intensivists struggling to care for critically ill COVID-19 patients by producing a series of engaging educational videos.
As the pandemic caused by the SARS-CoV-2 coronavirus has swept across the globe, general practitioners, emergency medicine specialists, hospitalists, and other physicians in hard-hit cities have been called upon to manage the care of patients with acute respiratory distress syndrome (ARDS). Many of these medical professionals have little or no training in ARDS. Even for those familiar with the syndrome, its presentation in the setting of COVID-19 challenges the usual understanding and requires a different approach.
The video series provides a valuable resource for healthcare professionals suddenly confronted with a new disease with poorly understood pathophysiology and rapidly changing treatment recommendations. The series includes basics of intubation and ventilation in the setting of a highly contagious disease and goes into greater detail on transport ventilation, airway pressure release ventilation, acute respiratory distress syndrome, and use of medications often needed by COVID-19 patients in intensive care. The videos can be found on the health.mil website.
CARDS vs. ARDS
ARDS presents as very rapidly progressing shortness of breath and low blood oxygen levels. Generally characterized by widespread inflammation of the lungs and reduced aerated lung size, ARDS is typically caused by pneumonia, sepsis, trauma, inhalation of lung-damaging substances, or near drowning. As it progresses, fluid accumulates in the alveoli, blocking oxygen from reaching the bloodstream. Some patients will develop scarring in the lungs or fibrosis; others may suffer pneumothorax or collapsed lung.
For many patients suffering from ARDS, mechanical ventilation is an essential, lifesaving treatment. But ventilation can be a double-edged sword: The pressure required to keep the lungs open and the blood oxygenated can sometimes cause catastrophic, even fatal, damage to the lung’s delicate tissues.
Striking the right balance has been challenging with COVID-19-related ARDS, also known as CARDS. Early reports indicated that more patients with pneumonia caused by the novel coronavirus required intensive care, more in intensive care needed mechanical ventilation, and more on ventilators died than in other kinds of ARDS. In fact, some studies indicate that mortality from CARDS is double that seen in traditional ARDS.1
The higher mortality rate associated with CARDS has prompted a closer look at the impact COVID-19 has on the lungs. That’s turned up some notable differences between CARDS and traditional ARDS.
“Unlike routinely encountered cases of ARDS, respiratory system compliance [in CARDS] remains relatively normal despite impressive hypoxemia, indicating flexible, gas-filled lungs until later and/or more advanced stages,” according to a recent editorial in Critical Care Medicine by John J. Marini, MD, of the University of Minnesota, in St. Paul.2
“This early flexibility explains why some hypoxemic and spontaneously breathing patients appear quite comfortable despite high ventilation requirements,” Marini said.
Other physicians have dubbed these paradoxical patients “happy hypoxics,” as they continue to hold conversation and appear otherwise healthy prior to examination despite having dangerously low oxygen levels. Some have compared the presentation of these patients in early CARDS to individuals with high-altitude pulmonary edema (HAPE), although the conclusions drawn from that comparison differ between prominent pulmonologists.
Different Approaches
Luciano Gattinoni, MD, of the department of Anesthesiology and Intensive Care at the Medical University of Göttingen, Germany, classified patients with simultaneous hypoxemia and compliant lungs as having the type L phenotype of COVID-19 pneumonia-induced ARDS. This type of respiratory failure also has low ventilation to perfusion ratio, low lung weight and low recruitability.3
About 30% of patients progress to the type H phenotype of COVID-19 ARDS, which more closely resembles conventional ARDS. Type H patients have high elastance, high right-to-left shunt, high lung weight, and high lung recruitability, according to Gattinoni.
Much remains unknown about the pathophysiology and progression of respiratory failure in COVID-19. Patients may deteriorate, moving from type L to type H, as a result of an interplay of the viral infection itself, the immune response to the infection, hemodynamic factors, and lung injury from ventilation.
Because of the differences between L phenotype patients or the “happy hypoxics” and patients with more traditional presentations of ARDS, a number of experts in the field have recommended using therapies that diverge from the ARDSNet protocol developed for classic ARDS.
The thought is that changing ventilator strategies might keep more patients from progressing to the more severe manifestations of the syndrome. Suggested strategies include using nasal cannula or continuous positive airway pressure (CPAP) or bilevel positive airway pressure machines for patients who respond to oxygen therapy and do not require intubation, although the latter two options increase the risk of aerosolization of particles and spread of infection.
Others have found that changing the ventilation approach even for patients with more severe lung injury can increase survivability. Extracorporeal membrane oxygenation (ECMO) has been used in some instances. ECMO oxygenates blood outside the body, reducing stress on lungs. ECMO is an expensive procedure, however, with its own complications, including bleeding and stroke. The equipment is also not widely available.
Another option is airway pressure release ventilation (APRV). APRV is a ventilatory mode that uses fairly high and sustained continuous positive pressure, combined with a short release phase that permits carbon dioxide removal. APRV allows the patient to breathe spontaneously throughout respiration, independent of the ventilator cycle.
“So far, we have had considerable success with APRV in our COVID patients,” said Josh Farkas, MD, a critical care and pulmonary disease physician, assistant professor at the University of Vermont Medical Center in Burlington, VT, and editor of the Pulmcrit blog. “This has allowed us to support and extubate several patients successfully, while avoiding paralysis, proning, deep sedation, inhaled pulmonary vasodilators, or ECMO.”
Using APRV as the initial ventilator mode rather than as salvage might be most useful, he noted. Typically patients find APRV more comfortable, so they require fewer medications.
“Patients typically can be weaned from 100% FiO2 to 50% FiO2 on APRV within six to 12 hours as they slowly recruit,” he noted, though those that do not respond within 12 to 24 hours should be moved to prone ventilation.
- ICNARC. ICNARC report on COVIC-19 in critical care. 29 May 2020.
- Marini JJ. “Dealing with the CARDS of COVID-19.” Critical Care Medicine. May 13, 2020. Online first. DOI: 10.1097/CCM.0000000000004427
- Gattinoni L. et al. COVID-19 pneumonia: different respiratory treatment for different phenotypes? Intensive Care Medicine. 2020 DOI: 10.1007/s00134-020-06033-2

