MINNEAPOLIS — Even though chronic lymphocytic leukemia is a disease of older adults, with median age of 68 years at diagnosis, clinical trials on chemo-immunotherapy agents rarely included patients of advanced age, according to a new study.
Noting the strong correlation between age and mortality in patients with CLL, the article in Geriatric Oncology pointed out that the median age of participants in those clinical trials tended to be 10 or more years younger than the average age of diagnosis.1
Researchers from the Minneapolis VA Health System and the University of Minnesota emphasized that is especially an issue now that ibrutinib and venetoclax have become first-line therapy in addition to chemo-immunotherapy and have been studied in older patients. Yet, they explained, not all patients can receive those agents, because of comorbidities or because of the limitless duration of therapy.
“For this reason, we have examined patterns of CLL treatment for up to five lines of therapy, focusing on older patients, in this retrospective analysis of a large patient series over a five-year period of time in the pre-ibrutinib/venetoclax era,” the authors wrote.
The study team used the VA Tumor Registry to identify 2,052 patients diagnosed with CLL from 2009 to 2013, collecting data from chart review on baseline demographics, laboratory and disease-related parameters at diagnosis, including bone marrow cytogenetics when available. Lymphocyte doubling time was determined, and cytogenetic testing included standard karyotyping or fluorescent in-situ hybridization techniques. Of the patients, 681 (33.2%) received therapy for CLL.
For the study, deletions in 17p and 11q were considered as poor risk cytogenetics, while deletion 13q was considered a favorable risk. Researchers defined overall survival as time from CLL diagnosis to death from any cause or date of last follow-up, if still alive. Patients were censored at last follow-up if listed as alive.
The researchers collected, up to a maximum of five lines of therapy, all treatment data, including agents administered, number of treatment cycles, timing of regimen initiation and therapeutic response (if available).
Patients were divided into five groups based upon their initial treatment:
-
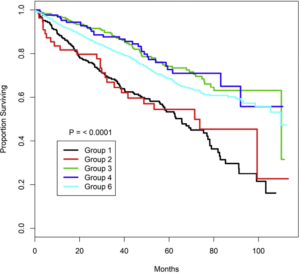 Steroids alone or with an alkylator, single-agent rituximab or chlorambucil-rituximab (Group 1);
Steroids alone or with an alkylator, single-agent rituximab or chlorambucil-rituximab (Group 1); -
Rituximab, cyclophosphamide, vincristine, prednisone (R-CVP) or rituximab, cyclophosphamide, doxorubicin, vincristine, prednisone (R-CHOP) (Group 2);
-
Single agent fludarabine, or in combination with rituximab, cyclophosphamide or both, or pentostatin, cyclophosphamide, and rituximab (referred to as fludarabine-based regimens) (Group 3);
-
Bendamustine and rituximab (Group 4); or
-
Other therapies including obinutuzumab alone or with chlorambucil, single agent methotrexate, lenalidomide alone or with corticosteroids, vincristine with corticosteroids or rituximab, and other varied combination regimens (Group 5).
The study also included patients receiving supportive care only.
Results indicated that the most commonly utilized regimens, involving 36.1% of treated patients, were steroids +/− rituximab +/− alkylators (Group 1), followed by fludarabine-based regimens (Group 3) at 34.2%. Treated patients ranged in age from 29 to 97, with a median of 68, and 34.7% were older than 70.
The median age of patients treated with steroids +/− rituximab +/− alkylators or R-CVP/R-CHOP (Groups 1, 2) was 72 and 71 years, respectively, although patients receiving fludarabine- or bendamustine-based regimens (Groups 3, 4) were about a decade younger—median 61 and 63 years, respectively.
Specifically, in Groups 1 and 2, 56.1% of patients were older than 70, compared to only 13.8% and 22.0% of those receiving fludarabine- or bendamustine-based regimens respectively (Groups 3, 4).
Among the untreated patients, meanwhile, nearly half, 49.7%, were older than 70.
“Prior to ibrutinib and venetoclax, there were minimal data on patterns of care in older patients with CLL, and a paucity of data still exists regarding patients not enrolled on clinical trials,” the authors noted. “While ibrutinib and venetoclax are now considered first line therapies, not all patients are eligible for these agents, due to potential cardiac and thrombophilic comorbidities, prolonged cytopenias, or because of the desire for time-limited therapy. Our study, an analysis of “real world” data, though with a marked male predominance and an emphasis on older patients, helps elucidate what clinicians are actually doing in this setting, where evidence regarding therapy sequencing is lacking.”
The study calculated that patients 70 or older had improved overall survival if they received bendamustine- or fludarabine-based regimens as compared to steroids +/− rituximab +/− alkylators, or R-CVP/R-CHOP, adding, “However, it is difficult to determine whether the improved survival was an effect of treatment choice or of this cohort having lower risk disease on aggregate. This observation may also be due to this group having a lower “physiologic age” than patients in other groups. Their physicians likely determined that they were fit enough to receive this more aggressive treatment.”
Overall, the authors said their study showed that older patients can receive aggressive CLL therapy.
“It is interesting to note that our population had an expected decrease in survival in patients with 17p deletions, but our patients with 11q deletions had similar overall survival to patients with normal 11q alleles,” according to the researchers. “Our patients with 13q deletions had improved survival as compared to others, which is consistent with the current understanding of this mutation’s impact.”
The report emphasized that chemotherapy still plays a key role in treatment of CLL and probably would continue to be important.
Since 2013, new agents such as ibrutinib and venetoclax have been investigated and are now first line treatments for CLL,” according to the study. “Yet despite these advances, chemotherapy continues to have a role in those ineligible for these new therapies due to comorbidities, desire for time-limited treatment and in the relapsed/refractory disease setting. Further, as we generate more data regarding long-term toxicities and outcomes from ibrutinib and venetoclax, chemotherapy may resume a more central role in CLL treatment.”
Nothing that their research identified trends in CLL therapy choices based upon age, as well as factors impacting use of subsequent therapies and outcomes with these treatments with an emphasis on older patients, the authors added, “Our findings may be of benefit in treatment decisions for patients outside of clinical trials, especially for patients whose baseline characteristics and treatment preferences preclude the use of newly approved agents.”
- Jacobsen AM, Gilbertson DT, Tarchand G, Morrison VA. Chemoimmunotherapy practice patterns in older patients with chronic lymphocytic leukemia: Impact of age and baseline characteristics on treatment choices. J Geriatr Oncol. 2020;11(1):134–140. doi:10.1016/j.jgo.2019.10.016

