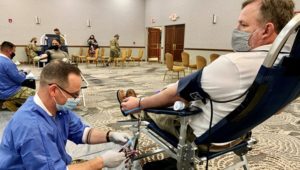
Army Sgt. Brett Knox with the Kendrick Memorial Blood Center, located outside Fort Gordon, GA, takes blood from Patrick Young, an employee at Winn Army Community Hospital, as a participant in the DoD COVID-19 Convalescent Plasma Program. Photo by Zach Rehnstrom
WASHINGTON — The DoD is on the attack against a wily and deadly enemy that has killed hundreds of thousands of Americans, devastated populations in cities, and destroyed significant segments of the economy.
Military experts have assumed command of the nation’s most aggressive response to the SARS-CoV-2, the virus that causes COVID-19, as vaccine developers, logistics experts, and engineers from across the armed forces bring their specialized experience and focus to Operation Warp Speed.
With a goal of distributing 300 million doses of a COVID-19 vaccine by January 1, 2021, Operation Warp Speed (OWS) is a massive undertaking designed to enable the country to regain some sense of normality in the face of a novel, deadly pathogen that has disrupted daily life in the U.S. and around the world. As the centerpiece of a broad strategy that includes multiple countermeasures against the virus including development, testing, and distribution of diagnostics and therapeutics, OWS draws on critical capabilities resident in the DoD and the Department of Health and Human Services.
The ambitious project is jointly chaired by Defense Secretary Mark Esper and HHS Secretary Alex Azar, but the DoD’s leadership extends to almost all parts of the ambitious project. In total, about two-thirds of the 90 named leaders in the OWS organizational chart obtained by STAT News come from the DoD.
HHS includes most of the organizations that have played public roles in combatting the virus, such as the national Centers for Disease Control and Prevention (CDC), the Food and Drug Administration (FDA), Biomedical Advanced Research and Development Authority (BARDA), the National Institutes of Health (NIH) and its prominent National Institute of Allergy and Infectious Diseases. While these organizations have deep expertise in disease prevention and treatment as well as awareness of public health resources in communities, they lack the raw manpower of the DoD.
“HHS was never manned to be able to simultaneously and as rapidly go through clinical trials, go through the development, go through the manufacturing, and then distribute six separate vaccines in a pandemic environment,” said Paul A. Ostrowski, the DoD’s chief of supply and distortion for OWS. “That is a Herculean task. What we bring is a bandwidth and the enablers to allow that to happen — not only for vaccines, but also for therapeutics.”
OWS focuses on five primary areas:
-
development and testing of vaccines;
-
development and testing of therapeutics;
-
development and testing of diagnostics;
-
supply production and distribution of vaccines, diagnostics and therapeutics; and
-
security and assurance of vaccine, diagnostic and therapeutic development, testing, supply production and distribution.
Massive Coordination Needs
The DoD’s contributions to OWS include managing contracts, building vaccine production facilities, enrolling participants in vaccine trials and more. The massive program involves coordination with dozens of private companies such as pharmaceutical companies, medical supply vendors, vaccine raw material suppliers, and transportation providers. The contracts for syringes and safety needles for administration of a vaccine alone totaled $104 million.
“Getting exactly what the government has paid for by each one of these particular companies is extremely important,” Ostrowski said. “[That] program manager and contracting experience and expertise is critical to our successful mission here at OWS.”
The Corps of Engineers and the Navy’s Construction Battalions (SeaBees) have weighed in on the effort as well. The two construction groups are building facilities that can accommodate the rapid production of millions of doses of vaccine in record time.
“The manufacturing capacity within the United States for vaccines . . . did not meet the amount of demand that we’re going to get with respect to this COVID pandemic,” Ostrowski noted. Some of those facilities are already in use, producing doses of potential vaccines even before they have completed clinical trials so that, if approved by the FDA, the vaccines would be ready for immediate distribution.
OWS selected six COVID-19 vaccine candidates for initial support and has funded four for phase 3 trials so far—NIAID/Moderna’s mRNA-1273, the University of Oxford/AsteraZeneca’s AZD1222, Pfizer/BioNTech’s BNT162, and Johnson & Johnson’s AD.26.COV2.S. Vaccines in development by Sanofi and GlaxoSmithKline are in phase 2 trials. The phase 3 clinical trials for each of the vaccines will require 30,000 or more participants.
“To have just one candidate vaccine in Phase 3 trials less than a year after a virus was first reported would be a remarkable accomplishment; to have four candidates at that stage is extraordinary,” said HHS Secretary Alex Azar. “By building a portfolio of candidate vaccines, Operation Warp Speed is maximizing the chances that we will have substantial supplies of a safe and effective vaccine—and maybe multiple vaccine options—by January 2021.”
Getting approved vaccines to communities across the country will pose its own challenges. “We have to deal with the difference between single doses and double doses,” said Paul Mango, deputy chief of staff for policy at HHS. “We also have to deal with different storage and transport requirements. So when you add all this up, there’s five or six major independent variables, and when you run the number of combinations that we’re planning for, it’s quite extraordinary.”
The DoD has tackled many of the logistical issues involved in distribution already, ensuring that any approved vaccine quickly and safely reaches hospitals, clinics, and pharmacies for administration. Now, Defense experts are addressing another issue that could arise if more than one of the current candidates gains approval—making sure that people who receive the first dose of a two-part vaccine receive the correct vaccine for the second dose regardless of where they go for the second shot. That will require enabling communication between different system’s vaccine tracking databases.
“What we’re in the process of doing is being able to help allow those different databases to talk with one another through a data link that we’re developing and testing as we speak,” Ostrowski said.
