3D medical animation still showing Irritable bowel syndrome and tenesmus in the pip. Source: Scientific Animations
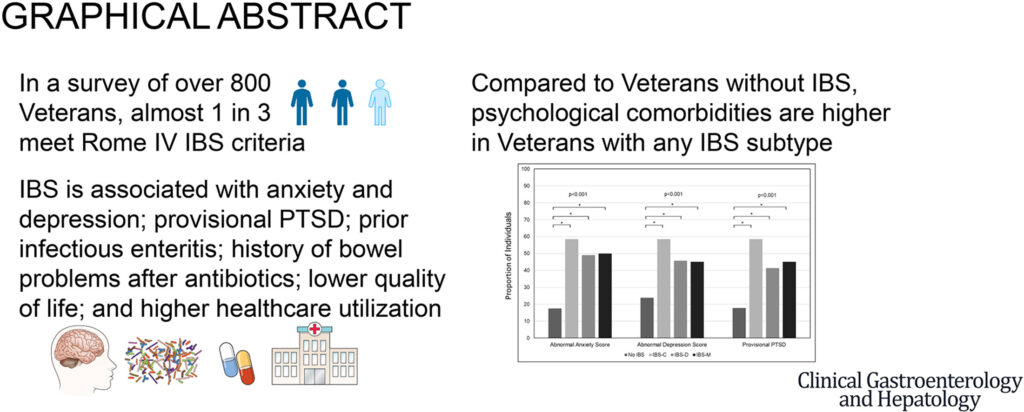
SEATTLE — Irritable bowel syndrome (IBS) is a syndrome characterized by abdominal pain and altered bowel habits. It is known as a disorder of gut-brain interaction due to dysregulation of the gut-brain axis (bidirectional signaling between the gut and the brain), which can be related to central and peripheral mechanisms and results in significant healthcare expenditures and reductions in health-related quality of life.
Patients with IBS commonly meet criteria for psychiatric conditions, and numerous studies have reported an association between psychological, physical or sexual trauma and diagnosis of IBS. Although most of these studies have focused on childhood trauma and abuse, others support an association between gastrointestinal (GI) symptoms and trauma when trauma is experienced later in life—such as deployment to a war zone and combat exposure.
Given links between trauma and IBS, research has begun to examine the relationship between IBS and PTSD among veterans. Yet much of the research to date has focused on whether patients meet criteria for IBS and has emphasized pain severity.
“We were interested in examining a broader range of gastrointestinal symptoms including abdominal/belly pain, gas/bloating, constipation and diarrhea in addition to the prevalence of irritable bowel syndrome among veterans,” said Kendra Kamp, RN, PhD, assistant professor in the University of Washington’s School of Nursing and author of a new study published in the Journal of Clinical Gastroenterology. The study provides insight into the relationship between gastrointestinal symptoms, PTSD severity, depression severity, and number of prior traumatic events reported.1
The study used data that was collected as part of a larger randomized control trial which was focused on behavioral interventions for veterans with PTSD, Kamp told U.S. Medicine. “This provided an opportunity to collect additional data on gastrointestinal symptoms.”
The primary inclusion criterion was for veterans who met the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria for PTSD for any reason (i.e., not limited to combat-related trauma). Veterans were excluded if they met any of the following criteria: substance use dependence disorder other than alcohol, alcohol use that posed a safety concern, high risk of suicide, psychotic disorder, mania, diagnoses of borderline or antisocial personality disorder documented in the electronic health record or a psychiatric admission in the past month. One hundred eighty-four veterans with a diagnosis of PTSD were included.
A diagnosis of IBS was assessed by the Rome III questionnaire, which assesses criteria over the past 12 weeks. Veterans completed questionnaires assessing gastrointestinal symptoms (Gastrointestinal Patient-Reported Outcome Measures Information Systems; PROMIS) and lifetime traumatic events. Multivariable regression analyses were performed to examine associations between gastrointestinal symptoms and the number of prior traumas reported PTSD severity, and depression symptom severity.
High Prevalence
The study found that 25% of veterans with PTSD in the study met Rome III criteria for IBS, which is higher than the prevalence in the United States. Commonly reported gastrointestinal symptoms included abdominal/belly pain (36%), diarrhea (21%), constipation (18%), and bloating/gas (17%).
Other notable findings included:
- The percentage of veterans with PTSD reporting abdominal/belly pain was greater than reported in a nationally representative survey of the U.S. population, which found abdominal pain in 24.8% of the sample in the past week.
- Rates of constipation, diarrhea and bloating/gas in the study were similar to those reported in a Nationally Representative Survey in the United States.
- Severity of PTSD was significantly associated with each of the GI symptoms of abdominal/belly pain, constipation, diarrhea and gas/bloating as well as meeting the criteria for IBS.
- Number of prior traumas was associated with gas/bloating and meeting
criteria for IBS. - Depression symptom severity was associated with GI symptoms of abdominal/belly and constipation as well as meeting criteria for IBS
“The evidence that PTSD is associated with an excess risk of IBS adds to a broader literature indicating that PTSD is associated with higher rates of other health problems, including coronary artery disease, asthma and arthritis,” the authors wrote.
“Our study highlights the importance of evaluating gastrointestinal symptoms among veterans with PTSD as well as providing appropriate referrals,” said Kamp, adding that “additional research is needed to better understand the overlap between gastrointestinal symptoms and PTSD.”
- Kearney DJ, Kamp KJ, Storms M, Simpson TL. Prevalence of Gastrointestinal Symptoms and Irritable Bowel Syndrome Among Individuals With Symptomatic Posttraumatic Stress Disorder. J Clin Gastroenterol. 2022 Aug 1;56(7):592-596. doi: 10.1097/MCG.0000000000001670. Epub 2022 Jan 28. PMID: 35089910.