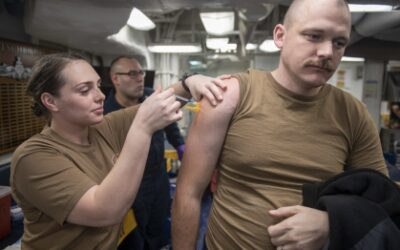
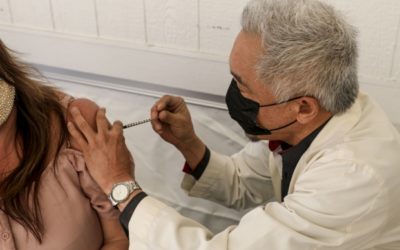
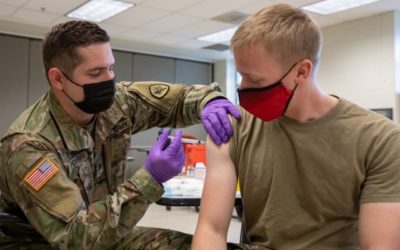
Although serious allergic reactions to mRNA vaccines are extremely rare, fear of them has driven hesitancy among some potential recipients. That especially has been the case when an adverse effect occurred after the first dose.
MHS Researchers Found Current Antibiotic Dosing Guidelines Adequate for Critically Ill Patients With Trauma, Burn
Critical illness caused by burn and sepsis doesn’t alter how the body processes piperacillin and tazobactam (pip-tazo), an antibiotic and beta-lactamase inhibitor drug combination
Low VHA COVID-19 Booster Rates Leave Veterans Vulnerable to Severe Cases
President Joe Biden, despite being 79 years old, had a mild case of COVID-19. The primary explanation for why he escaped severe symptoms is that he was not only vaccinated, but double-boosted.
‘Pan-Coronavirus’ Vaccine Developed by Army Research Shows Promise
Based on recent preclinical study results, the Spike Ferritin Nanoparticle (SpFN) COVID-19 vaccine is showing significant promise.
National Guard Pandemic Response Proves Motto ‘Always Ready, Always There’
For more than two years, the National Guard has risen to the challenges posed by COVID-19 as the pandemic has disrupted lives, supply chains, health care, education and more.
VA Studies Continue to Demonstrate High COVID-19 Vaccine Effectiveness
From the time the COVID-19 mRNA vaccines became available in late 2020, VA studies have been crucial to understanding their effectiveness in real life.
Ann Arbor VAMC Rapidly Stands Up Monoclonal Antibody Treatment Service
As emergency departments around the country struggled to get through the day during the recurrent surges of the COVID-19 pandemic, the emergency medicine team at the LTC Charles S. Kettles VAMC here did something extraordinary—they sought out more patients to treat.
Shingles Vaccination Rates Struggle to Improve at VA
Efforts to promote use of a vaccine against herpes zoster, commonly called shingles, have been fraught with difficulty.
How Deployed Military Personnel Viewed COVID-19 Vaccination
To better understand vaccine hesitancy related to COVID-19 shots, a study recently looked at how likely deployed military personnel is to be vaccinated.
Receipt of Multiple Vaccines Lessens Dementia Risk
Are older adults who receive both herpes zoster (HZ) and a tetanus, diphtheria, pertussis (Tdap) vaccine less likely to experience cognitive issues than seniors who receive only one or the other vaccine?
Moderna COVID-19 Vaccine Proves More Effective Than Similar Pfizer Product
While both of the messenger RNA vaccines used in the United States work very well, a new VA study found that, in a head-to-head comparison, the Moderna product is more effective than the Pfizer-BioNTech product.
VA Seeks to Change Initial Concerns About COVID-19 Vaccines Into Acceptance
Early in 2021, more than one-fourth of veterans responding to a survey said they were concerned about getting a COVID-19 vaccine. The VA has worked steadily since then to change their minds.
Military Begins Discharges of Servicemembers Refusing COVID-19 Vaccines
Most active-duty U.S. servicemembers had been vaccinated against COVID-19 by mid-December, when the Army set its deadline.
Which Cancer Patients Get Most Protection From COVID-19 Vaccines?
With new variants popping up and steady occurrence of breakthrough infections, the question of the effectiveness of SARS-CoV-2 vaccination in patients with cancer has not really been answered until now.
DoD Will Provide Medical Workers to Help Civilian Hospitals Fight Omicron
In response to the surge of COVID-19 cases related to the omicron variant, President Joe Biden said that an additional 1,000 military medical personnel would be available to aid civilian hospitals in the United States by early this year.
VA Played Critical Role in Successful Roll-Out of COVID-19 Vaccines
When the COVID-19 vaccines rolled out last winter, a unique partnership between the VHA and other federal agencies provided the first real-world evidence—outside of clinical trials—of how well the vaccines were working.
Death Rate Increases for VA Patients Lagged Community Levels Last Year
Despite older age and more potentially dangerous comorbidities, veterans receiving VA care fared better last year than those treated in community healthcare systems during the COVID-19 pandemic, according to a new study.
Nearly All VA Employees Comply with Federal COVID-19 Vaccine Requirements
Nearly all, 98%, of VA employees facing a COVID-19 vaccination requirement have had at least one dose of vaccine or have requested an exception or extension, according to White House data released just before Thanksgiving.
As Deadlines Neared, DoD Moves Toward Fully Vaccinating Active-Duty Troops
The DoD is moving steadily toward its goal of vaccinating all military personnel. By early November, 97% of the DoD’s active-duty force had received at least one dose of COVID-19 vaccine.
Only About Half of ASCVD Patients Get Influenza Vaccines
Only about half of U.S. patients with atherosclerotic cardiovascular disease receive annual influenza vaccine, and the rate is lower among Black and Hispanic patients than white ones.
VA Study Establishes Link Between Flu Infection, Acute Myocardial Infarction
Previous studies have established an association between laboratory-confirmed influenza infection (LCI) and hospitalization for acute myocardial infarction (AMI).
Kidney Injury Gauged in VA Influenza, COVID-19 Patients
COVID-19 is often compared to other respiratory viral illnesses, but few of those comparisons contrast the virus’ varying effect on kidney health and function.
Native Americans Have the Highest U.S. COVID-19 Vaccination Rates
Native Americans, a category including American Indians and Alaska natives, have consistently had the best COVID-19 vaccination rates in the United States since the shots became available in early 2021, according to the national Centers for Disease Control and Prevention.
Disparities Fueled Outbreaks of COVID-19 Among Native Americans
From the start of the pandemic, American Indians and Alaskan Natives have been disproportionately impacted by the virus. New data released last month by Johns Hopkins University (JHU) helps visualize that disparity, which has been blamed on a higher rate of preexisting conditions and poorer health infrastructure.
mAb Therapies Effective Against Severe COVID-19 in Native American Cohort
Monoclonal antibody (mAb) therapies were highly effective against COVID-19 in a recent study of Native Americans — a group that has been underrepresented in clinical trials for COVID-19 therapies despite being at greater risk for severe disease.
Patients With Uncontrolled HIV Face Higher Risk of Sudden Cardiac Death
A new veterans study underscored the critical need for viral suppression and heart disease risk factor modification among HIV patients. Researchers determined that those with sustained viremia or low CD4 cell counts had an excess risk of sudden death.
OIG: Lack of Planning Made Illinois CLC COVID-19 Outbreak Worse
From almost the very start of the pandemic, nursing homes and long-termcare facilities proved to be particularly vulnerable to the virus. The close quarters combined with elderly patients suffering from preexisting illnesses resulted in a number of outbreaks and a much higher death rate than the general population.
Immunologic Resistance Used to Predict COVID-19 Outcomes in Veterans
Is it possible to predict which COVID-19 patients will advance to severe disease? A new study involving VA researchers suggested that the answer is “yes,” using the concept of immunologic resilience.
Military Sets Deadlines for Receipt of Mandatory COVID-19 Vaccine
By mid-December, all U.S. active-duty servicemembers will either be vaccinated against COVID-19 or have received an approved exemption from their service branch.
Patients With Uncontrolled HIV Face Higher Risk of Sudden Cardiac Death
A new veterans study underscored the critical need for viral suppression and heart disease risk factor modification among HIV patients. Researchers determined that those with sustained viremia or low CD4 cell counts had an excess risk of sudden death.