WASHINGTON–Despite intense scrutiny of wait times for veterans seeking VA care over the last three years, a new study pointed out that delays in the private sector weren’t statistically less in 2014 and that, possibly because of the focus, wait times now are significantly shorter for the VA compared to private-sector healthcare facilities.
“In 2014, reports indicated that veterans were waiting too long for care and that scheduling data may have been manipulated at a United States Department of Veterans Affairs (VA) facility in Phoenix, Arizona,” according to the study in JAMA Network Open. “This incident damaged the VA’s credibility and created a public perception regarding the VA health care system’s inability to see patients in a timely manner.”1
VA researchers and colleagues noted that the agency has sought to improve access, adding, “There is evidence suggesting that these efforts have improved access to care, including reports that 22% of VA patients are now seen on the same day as the requested appointment. Despite these efforts, the adequacy of access to VA care remains unclear.”
Their cross-sectional study of wait-time data from VA facilities and private sector hospitals in primary care, dermatology, cardiology and orthopedics from 15 major metropolitan areas ultimately found that wait times remained unchanged between 2014 to 2017 in private-sector facilities but improved at the VA, surpassing access in the private sector for three of the four specialties evaluated.
“Since 2014, VA has made a concerted, transparent effort to improve access to care,” VA Secretary Robert Wilkie noted in a press statement. “This study affirms that VA has made notable progress in improving access in primary care, and other key specialty care areas.”
The study might raise questions, however, about the need for some provisions of the Mission Act, which was signed into law to give veterans more efficient access to healthcare. One of the authors was David Shulkin, MD, who was ousted as VA secretary last year by President Donald Trump at least partly because Shulkin was a vocal opponents of any moves toward privatization of VA care.
The JAMA Network Open study compared new appointment wait times at VAMCs with wait-time data for primary care, dermatology, cardiology or orthopedics at VA medical centers in 15 major metropolitan areas, with private sector comparison data coming from a published survey using a “secret shopper” approach.
In the study, secondary analyses focused on the change in overall and unique patients seen in the entire VA system, as well as patient satisfaction survey measures of care access between 2014 and 2017.
The primary outcome was patient wait time, with those determined directly from patient scheduling at the VA and drawn from Merritt Hawkins surveys in the private sector.
Results indicated that, compared to the private sector, overall mean VA wait times for new appointments in 2014 were similar (mean [SD] wait time, 18.7 [7.9] days PS vs 22.5 [7.3] days VA; P = .20).
Shorter Waits
In fact, the authors emphasized, VA wait times in 2014 were similar to those in the private sector across most specialties and regions. In 2017, on the other hand, overall wait times for new appointments in the VA were shorter than in the private sector.
Specifically, wait times were shorter at the VA in:
- primary care (mean [SD], 20.0 [10.4] vs 40.7 [35.0] days; P = .005),
- dermatology (mean [SD], 15.6 [12.2] vs 32.6 [16.5] days; P < .001), and
- cardiology (mean [SD], 15.3 [12.6] vs 22.8 [10.1] days; P = .04).
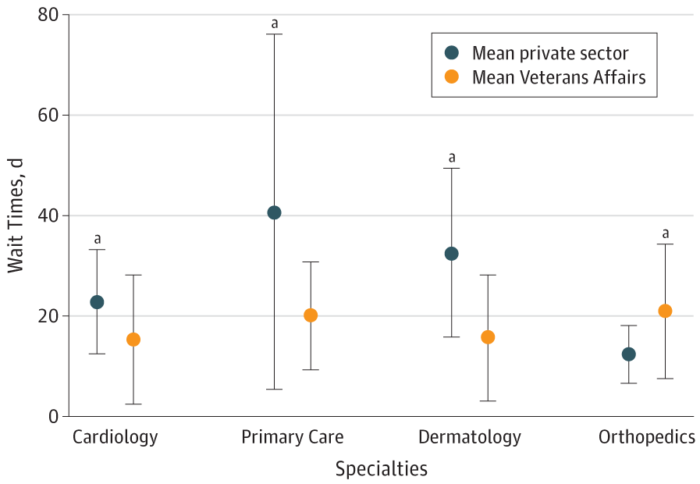
The study reported that wait times for orthopedics remained longer in the VA than the private sector (mean [SD], 20.9 [13.3] vs. 12.4 [5.5] days; P = .01) but improved significantly between 2014 and 2017 in the VA for orthopedics vs. the private sector, which saw no significant change—mean wait times increased 1.5 days in the private sector, while decreasing 5.4 days at the VA.
At the same time, secondary analysis revealed an increase in the number of unique patients seen and appointment encounters in the VA between 2014 and 2017—about 5 million to 5.1 million and 15.5 million to 17.3 million, respectively.
Wait times varied by geographic region, however. While, in 2014, VAMC in the Dallas, Miami and Portland, OR, areas had significantly longer wait times than the private sector—20.6 vs. 10.3, 22.3 vs. 13.8 and 42.3 vs. 15.5, respectively, wait times were similar compared to the VA for the other 12 regions.
In 2017, however, no metropolitan areas showed statistically significant differences in wait times between the private sector and VA, with analysis suggesting that the estimated mean wait times were actually shorter at the VA for 22 of the 30 metropolitan areas.
Study authors also documented improvement in patient satisfaction measures of access across the VA, which increased by 1.4% for specialty care, 3.0% for routine primary care and 4.0% for urgent primary care.
“Although wait times in the VA and PS appeared to be similar in 2014, there have been interval improvements in VA wait times since then, while wait times in the [private sector] appear to be static,” the researchers wrote. “These findings suggest that access to care within the VA has improved over time.”
They added that their data suggested “VA initiatives, rather than changes to the overall health services market,” led to the improvements.
A related commentary from Peter J. Kaboli, MD, MS, of the Iowa City Veterans Affairs Healthcare System and the University of Iowa, both in Iowa City, IA, and Stephan D. Fihn, MD, MPH, deputy editor of the journal and on the faculty of the University of Washington, Seattle, pointed out some of the study’s limitations.2
For example, the commentators noted that wait times were only studied for new patients, not pre-existing ones, explaining, “Favoring new patients may be at the expense of access for existing patients. In this era of expanding virtual care, focusing solely on in-person visits provides a distorted perspective of access, implying that only a face-to-face encounter can address the needs of patients. Health systems across the globe are moving away from that construct”
Kaboli and Fihn also described how Consumer Assessment of Healthcare Providers & Systems survey scores, which measure member perceptions of their health plan and the quality of the healthcare service they receive, remain lower for VA compared to Medicare, for example.
“The discordance between measured wait-time metrics and patient-perceived access may be due, in part, to continuing negative coverage of the VA in the press, as well as public proclamations that create unrealistic expectations (e.g., universal access to same-day appointments) that may not have been fully met by increased capacity to deliver such timely care,” they explained.
Despite that, the commentary concluded that “the 7 million veterans who receive care from the VA seem able to obtain routine and urgent care in a time frame that is on par for other Americans despite increasing demand, although there are and always will be exceptions. As resources in the VA are increasingly diverted to purchase care in the community, it remains to be seen if access to health care services can be maintained while access in the private sector continues to deteriorate. To understand how access to care in the VA and the community evolves, more reliable and valid metrics of access to care will be essential.”
1. Penn M, Bhatnagar S, Kuy S, Lieberman S, Elnahal S, Clancy C, Shulkin D. Comparison of Wait Times for New Patients Between the Private Sector and United States Department of Veterans Affairs Medical Centers. JAMA Netw Open. 2019 Jan 4;2(1):e187096. doi: 0.1001/jamanetworkopen.2018.7096. PubMed PMID: 30657532.
2. Kaboli PJ, Fihn SD. Waiting for Care in Veterans Affairs Health Care Facilities and Elsewhere. JAMA Netw Open. 2019 Jan 4;2(1):e187079. doi: 10.1001/jamanetworkopen.2018.7079. PubMed PMID: 30657527.
