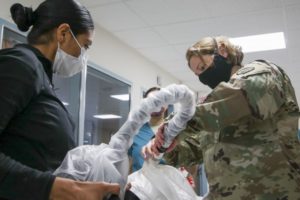
Medical personnel at Landstuhl Regional Medical Center in Germany familiarize themselves with the Powered Air-Purifying Respirator System, to increase safety while caring for COVID-19 patients. Devices like continuous glucose monitors help limit contact. Army photo by Marcy Sanchez
OMAHA, NE — COVID-19 and diabetes have proven to be a deadly combination. For patients infected with the novel coronavirus, diabetes more than doubles the odds of death. For healthcare workers, the need to closely monitor glucose levels and administer insulin or other medications creates additional exposure to a virulent pathogen.
Multiple studies have found that 20% to 35% of COVID-19 patients in intensive care have diabetes. To complicate issues, uncontrolled hyperglycemia is associated with longer hospital stays, while many of the drugs used to treat COVID-19 can increase blood sugar levels. Further, research indicates that the novel coronavirus can also trigger new onset diabetes.
“Much has been written about the treatment of patients with COVID-19 in general, but little guidance has been provided to clinicians on how to treat their patients with diabetes,” said Andjela Drincic, MD, professor in the department of Internal Medicine, Division of Division of Diabetes, Endocrine and Metabolism at the University of Nebraska in Omaha, Neb. “And yet, hyperglycemia in this population is rampant and difficult to treat.”
Drinicic and colleagues from the National Institutes of Health and major academic medical centers across the country recently published guidelines that outline a pragmatic approach to management of patients with high blood glucose levels who are hospitalized with COVID-19.1
Standard recommendations for managing hyperglycemic hospitalized patients call for at least four capillary blood glucose measurements per day using fingersticks, portable glucose monitors for patients receiving insulin injections and hourly tests for those on IV insulin. Hospitals experiencing a surge of patients with the coronavirus often lack the personnel and protective equipment needed to safely maintain such frequent monitoring at bedside.
“These healthcare providers are at risk for contracting COVID-19, and while glycemic management in the hospital improves patient outcomes, it also intensifies the amount of time with direct patient contact,” noted lead author Mary T. Korytkowski, MD, of the University of Pittsburgh School of Medicine in Pittsburgh.
Yet, reducing the number of blood glucose checks can be particularly dangerous in the current environment. “It is important to note that insulin requirements can vary on a daily if not hourly basis in patients with critical COVID-19 infections where there is variability in insulin sensitivity over the course of the illness,” the authors wrote. Wide fluctuations in insulin requirements in these patients can be exacerbated by medications, especially corticosteroids and hydroxychloroquine, and impaired kidney function prior to or as a result of their coronavirus infection.
Generally, patients who are taking non-insulin medications to manage their diabetes at the time of admission should be switched to insulin and patients with newly recognized hyperglycemia should initiate insulin to avoid a range of adverse effects. In some cases, the dipeptidyl peptidase 4 inhibitors (DPP4i) sitagliptin and linagliptin could be considered in patients with mild, recovering cases.
Continuous Glucose Monitoring
With insulin advised for most COVID-19 patients with diabetes, how can hard-hit hospitals manage appropriate monitoring? The authors note that some patients may be able to continue self-monitoring blood glucose levels, reducing the burden of healthcare workers. This group could include non-critically ill patients comfortable with performing regular fingerpricks and using their own or a hospital-provided blood glucose meter as well as those who enter the hospital with their own continuous glucose monitoring (CGM) devices.
In April, the U.S. Food and Drug Administration announced that it would not object to in-hospital use of continuous glucose monitors to manage glycemic issues in COVID-19 patients, which had previously been cleared for use only in ambulatory and research settings.
The FDA decision has enabled many hospitals around the country to use the two CGM devices that do not require regular calibration against capillary blood glucose measures and enable remote monitoring of blood glucose data for up to 14 days. The manufacturers of both devices have made their CGMs available at a reduced cost during the pandemic.
Scripps Health in San Diego, Calif., is one system that chose to use the devices. “By taking advantage of the opportunity allowed by the FDA, we are bringing down barriers that normally would have impeded the broader use of this technology in hospitals and, instead, rapidly yet safely bringing it to the bedside where it will benefit both patients and staff members,” Scripps Whittier Diabetes Institute lead research scientist Addie Fortmann, PhD, said.
Scripps Whittier has been using CGM in a clinical study for five years. Preliminary results demonstrated that the devices were safe and feasible to use in a hospital environment and were associated with trends toward better glycemic control.
Rush University Medical Center in Chicago also reported good results in its early use of CGM during the pandemic. Raisa Kazlauskaite, MD, MS, director of the diabetes technology program at Rush University and associate professor at Rush Medical College, observed that the devices not only reduced demands on nursing staff, they improved patient safety by providing a fuller picture of a blood glucose levels over the course of a day. The greater frequency of measurements reduced the risk of undetected hypoglycemic or hyperglycemic episodes.
Francsco J. Pasquel, MD, MPH, a physician at Emory Hospital in Atlanta, noted that the devices were particularly valuable for intensive care patients who must maintain glucose levels in a narrow range while on IV insulin. In this setting and others where CGM indicates the need for adjustment in insulin doses or glucose levels are rapidly changing, the manufacturers recommend validating results with point of care capillary blood glucose measurements.
Pasquel, who co-authored an article on implementation on CGM in hospitals during the pandemic with colleagues at Emory and other leading medical schools as well as physicians at the Baltimore and Atlanta VAMCs, also noted that CGM would be useful for patients on other floors as well, including patients on steroids and those who require medical nutrition therapy.2
-
Korytkowski M, Antinori-Lent K, Drincic A, et al. A Pragmatic Approach to Inpatient Diabetes Management during the COVID-19 Pandemic. J Clin Endocrinol Metab. 2020;105(9):dgaa342. doi:10.1210/clinem/dgaa342
-
Galindo RJ, Aleppo G, Klonoff DC, et al. Implementation of Continuous Glucose Monitoring in the Hospital: Emergent Considerations for Remote Glucose Monitoring During the COVID-19 Pandemic. Journal of Diabetes Science and Technology. 2020;14(4):822-832. doi:10.1177/1932296820932903
