WASHINGTON—With the number of veterans being diagnosed with hepatocellular carcinoma continuing to rise, the VA has implemented several new initiatives to improve outcomes for patients with this aggressive cancer.
The most common type of liver cancer, HCC is the third-leading cause of cancer-related death worldwide. In recent years, most kinds of cancer have seen significant drops in incidence and mortality rates in the United States, but hepatocellular carcinoma remains an outlier.
Nationally, new diagnoses of liver cancer rose 38% between 2003 and 2012, and the number of deaths increased 56% in the same period, according to the national Centers for Disease Control and Prevention. The upward trend accelerated over time, with the incidence rate rising an average of 2.3% per year from 2008 to 2013 and the mortality rate increasing an average of 2.8% per year for men and 3.4% for women.
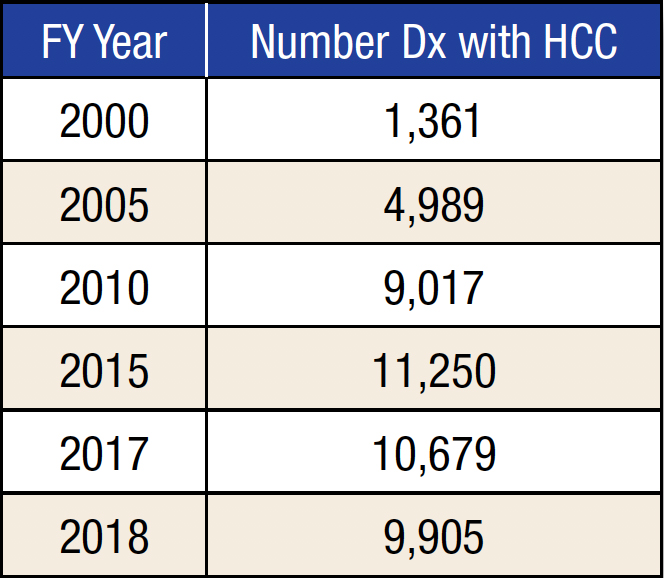
No healthcare system has seen the impact of the dramatic rise in HCC more clearly than the VA. In 2000, the VA had 1,361 patients diagnosed with the disease. By 2005, the number of veterans diagnosed with HCC had more than tripled to 4,989, according to the VA. By 2015, the number had doubled again, reaching 11,250. The number of veterans with HCC receiving care declined slightly to 9,905 in 2018 but is expected to resume its upward trend.
“HCC is different from most other cancers. Where the numbers for lung cancer, for instance, have remained relatively stable, HCC is skyrocketing now because of fatty liver disease,” said David Ross, MD, PhD, MBI, national director of the VA’s HIV, Hepatitis, and Related Conditions Programs and associate clinical professor of medicine at the George Washington University School of Medicine and Health Sciences in Washington.
A ‘Perfect Storm’
The largely male, baby boomer demographics of veterans who receive care through the VA apparently created a “perfect storm” for HCC. The cancer affects men at twice the rate seen in women, and chronic infection with the hepatitis C virus poses the highest risk of HCC for patients in the United States. Approximately 75% of U.S. cases of hepatitis C are found in individuals born between 1945 and 1965, a cohort with five times the risk of the infection compared to other age groups. As of 2016, approximately 180,000 veterans had been diagnosed with chronic hepatitis C infection.
A number of other factors increase the risk of HCC, and many of them also occur disproportionately in veterans, including diabetes, metabolic syndrome, obesity, alcohol use disorder and nonalcoholic fatty liver disease. Because of the elevated risk of HCC in its patient population, the VA has adopted a number of processes designed to identify and monitor those at greatest risk, standardize diagnosis and better manage treatment.
Screening for and treatment of hepatitis C have formed the cornerstone of VA’s HCC prevention efforts. With HCV nearly eliminated in the VA, new questions have arisen about how else to stem the rising tide of liver cancer.
“We need to continue to follow patients who have cirrhosis or other conditions that increase the risk of HCC like problem drinking or hepatitis B or nonalcoholic fatty liver disease,” Ross told U.S. Medicine.
Eighty percent of individuals diagnosed with HCC have cirrhosis, and the presence of cirrhosis in individuals with known risk factors can increase their risk of developing HCC between eight-and 25-fold, according to the American Association for the Study of Liver Disease. Consequently, the AASLD recommends surveillance using ultrasound with or without AFP every six months for adults with cirrhosis who are eligible for HCC treatment, a protocol followed by the VA.
Screening Questions
Questions about the need for such frequent screening remain, however. “There is not a randomized controlled trial showing that surveillance for liver cancer prolongs life,” Ross noted.
“There is a lack of high quality data,” agreed Fasiha Kanwal, MD, MSHS, an investigator in the Clinical Epidemiology & Comparative Effectiveness Program at the Center for Innovations in Quality, Effectiveness and Safety at the Michael E. DeBakey VAMC, chief of the Gastroenterology and Hepatology Section at the Baylor College of Medicine, both in Houston, and editor-in-chief of Clinical Gastroenterology and Hepatology.
“As a clinician who cares for these patients, though, we know that finding liver cancer early on will prolong life” Kanwal said. “And, it’s hard to randomize screening; patients want it.”
VA researchers have developed a number of new models for determining who would benefit most from ongoing surveillance. “The models revolve on cirrhosis or no cirrhosis. If no cirrhosis, does the patient have other risks? Alcohol use could be a factor,” Kanwal noted.
Particularly for patients for whom ongoing monitoring is clearly appropriate, “it’s not enough to do surveillance,” Ross added. “We have to move quickly, if we find something to evaluate. Not everything is liver cancer. In the majority of cases, if we find a lesion, we can make a decision without doing a biopsy.”
That’s possible because most cases of HCC now are diagnosed using radiology, Kanwal said. Imaging allows physicians and patients to avoid painful liver biopsies, which can cause dangerous bleeding and other complications.
In an effort to avoid delays in treatment and to standardize the technical aspects of diagnosis, imaging and management, the VA held a meeting of liver experts in March at the Miami VAMC. The goal is that “every VISN/VAMC uses the same optimized way to image and interpret liver lesions,” Ross explained.
Once HCC is diagnosed, information about the liver lesion goes into the patient record and a registry that can be viewed across the VA.
Nationwide access to the information makes assessing risks and next steps easier. “We have tumor boards set up in a large number of VAMCs already, and we’re on track to setting them up for every center,” Ross noted.
The tumor boards gather multidisciplinary teams of experts to evaluate what’s best for the particular patient. “Liver cancer can be cut out, or we could use radiation or chemotherapy. It all depends on the specifics,” he said.
The VA’s initiatives to better manage liver disease and HCC have already made a notable difference. They have reduced the time from diagnosis to treatment from three months to four weeks, Ross noted, “which makes a difference in whether patients live or die from this cancer. It’s been an incredible success so far.”
