BESTHESDA, MD—For traumatic musculoskeletal injuries, the Military Health System (MHS) provides cutting-edge care as it continues to pioneer new techniques to preserve limbs and restore function. For more mundane, yet frequently disabling injuries, both the VA and DoD rely on data-driven therapies and innovation to repair damage and minimize pain.
“Military orthopedic surgeons have more experience dealing with traumatic injuries than any other healthcare system,” said Marvin Helgeson, MD, chief of orthopedics at Walter Reed National Military Medical Center in Bethesda, MD. “As a profession, that’s our niche.”
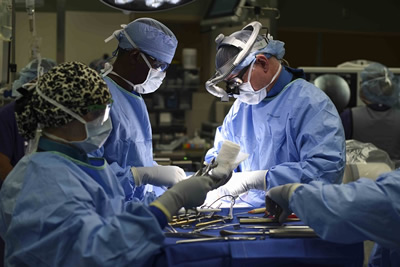
Air Force Col. Edward Anderson, MD, 99th Medical Group orthopedic spine surgeon, performs a lumbar microdiscectomy surgery at Nellis Air Force Base, NV. A lumbar microdiscectomy surgery is performed to remove a portion of a herniated disc in the lower back. Air Force photo by Airman 1st Class Andrew D. Sarver
The DoD has focused on streamlining “the reconstructive ladder from point of injury to restoring function,” Helgeson told U.S. Medicine.
Efficiently delivering servicemembers from where they incurred the injury to the initial level of care is the first step. Once there, “we take a multidisciplinary approach to cleaning wounds and stabilizing fractures,” Helgeson said.
For warriors who have sustained traumatic limb loss or are at risk of amputation, minimizing the risk of infection is paramount. “Musculoskeletal infections frequently complicate the clinical course of combat-injured patients with traumatic amputations and limb-threatening wounds,” according to a recent review of musculoskeletal injuries in the U.S. military.1 “Infectious complications range in severity from cellulitis, requiring only antibiotic therapy, to deep infection requiring surgical debridement.”
Because physicians within the MHS see many more of these injuries, “we lead the community in research in debridement and closure techniques, as well as in reconstructing tissue to optimize function,” Helgeson noted. Orthopedic, plastic and trauma surgeons work together to help injured service members achieve the best possible results, he added.
Walter Reed has developed two unique procedures to maximize use and minimize issues associated with prosthetics for amputees. Osseointegration addresses the difficulties created by the socket required for attachment of most prosthetics. For leg prosthetics, the socket transfers the force of the prosthetic foot hitting the ground to the skin, soft tissues and muscles before reaching the remaining bone.
The wear and tear on the skin and soft tissue is particularly problematic for battle-injured amputees who are more likely to have had split thickness skin grafts to preserve maximum limb length, but are more susceptible to ulceration, according to Walter Reed. Heterotopic ossification or bone formation in soft tissues of injured limbs, which occurs in up to 91% of traumatic amputations, also contributes to ulceration, pain, and nerve damage with traditional prosthetics.
The new procedure entails implanting a titanium peg into the femur or humerus to which an abutment that goes through the skin is attached. The external prosthesis then directly attaches to the abutment, eliminating the need for a socket. “We have done this procedure in 20 to 30 patients and all have able to maintain their prostheses,” Helgeson said.
Patients also experience an improved range of motion, better ambulation, and greater sensory awareness of the limb, which leads to more natural gait.2
The second advance is targeted muscle reinnervation, which can preemptively avoid pain from neuromas and phantom limb pain by surgically transferring amputated nerves to motor nerves in nearby muscles at the time of amputation.3 In addition, it “allows more function by being able to recruit muscle fiber more actively for amputees,” Helgeson added. The procedure also enables more intuitive control and an expanded range of motion for prosthetics.
Beyond Battlefield Injuries
Both the DoD and the VA have made significant investments in improving care and outcomes for service members or veterans who have experienced more common, non-combat-related injuries that lead to low-back pain and anterior cruciate ligament (ACL) ruptures.
Broadly speaking, VA/DoD guidelines encourage patients and physicians to try a wide range of interventions before resorting to surgery for back pain. “In the low-back realm, spine surgery as a whole gets a negative rap sometimes. In the civilian sector, there is evidence that there is too much surgery” with too little benefit, Helgeson said.
“Discectomies classically do well and patients who have them tend to stay on active duty. But reherniation happens in about 5% of cases, though we have no good studies that correlate reherniation to technical aspects of the surgery,” he observed. “It may be the manner in which you remove the disc and tissue around it, but no one has been able to prove that. In the meantime, we don’t want to miss the short-term outcomes because if something you do makes them undeployable for a year, they won’t be in the military.”
Other surgeries provide no simpler answers. “For cervical spine one- or two-level fusion or disc replacement, there are more questions about what happens 10 to 20 years down the road, whether it leads to degeneration,” he noted. “We don’t know if the best option is to fuse someone in the long-term because of problems with healing and adjacent damage. And only about half of patients stay on active duty after fusion.”
The advances seen in cervical spine options have not been paralleled in the lumbar region, Helgeson noted. “We’ve been on the leading edge for the last 15 years with cervical disc arthroplasty and patients have done very well. In the lumbar spine, we were in leading trials, but lumbar spine arthroplasty has not been proven to preserve motion as well as cervical.”
Walter Reed has adopted minimally invasive techniques as they have been developed. Those approaches may be especially suitable for the relatively young and healthy active duty population, which has a unique profile. Most back surgery patients have pain resulting from age-related degeneration.
The VA sees more of that older cohort as well as younger veterans who sustained injuries that led to ongoing back pain. Like DoD, VA focuses on providing a range of service to address pain, including surgery.
“Patients are choosing to be proactive about seeking musculoskeletal evaluation earlier rather than simply masking the pain with opiates. By seeking care earlier, we can intervene with non-surgical methods earlier as well, which tend to help,” said Alan Dang, MD, orthopedic attending at the San Francisco VAMC.
“There are multiple new techniques and technologies that are advancing the field of spine care, including endoscopic approaches for decompression,” Sanjog Pangarkar, MD, Physical Medicine and Rehabilitation, Greater Los Angeles VAMC, told U.S. Medicine. “In addition, certain lumbar surgery approaches such as OLIF [oblique lateral lumbar interbody fusion], are muscle sparing and allow faster recovery times.”
The VA also offer radiofrequency ablation for back pain, sometimes called “laser surgery,” as well as very complex multiday, staged spinal fusion surgeries, 3D printed titanium spine implants, robotic surgery, and computer navigation for complex cases, Dang said. “Any surgery that has strong evidence for use and, if applicable, is FDA cleared or approved is available at the VA,” he noted.
More recently, the San Francisco VA has used 3D patient-specific printed models created in-house to plan surgery and communicate with the surgical team and patient, Dang added. The cost can be less than a pair of sterile gloves and production takes less than 24 hours.
VA has also developed more intensive interdisciplinary pain programs than any other system, including cognitive behavior therapy, aquatic and physical therapy, acupuncture, yoga, tai chi, and other non-pharmacological, non-surgical techniques to help veterans “restore functioning and regain a sense of purpose,” said Jennifer L. Murphy, PhD, national cognitive behavioral therapy for chronic pain master trainer at the Tampa VAMC.
ACL Repairs
With ACL tears 10 times more common among active duty forces than civilians, military orthopedic surgeons have had abundant opportunity to study the injury and techniques for repair. “DoD is very interested in musculoskeletal injuries such as ACL ruptures because it’s one of the most common reasons for individuals to be not ready for deployment,” Helgeson said.
“Our sports-related surgeons do an incredible amount of volume,” he added. That allows the DoD to “critically assess long-term outcomes and whether specific technical aspects have an impact. Does ACL surgery result in recurrence or long-term stability or increase the risk of osteoarthritis? If so, is that outcome procedure specific?”
Continual evaluation of results and refinement of procedures keep “our folks always at the leading edge,” Helgeson said. “There is a lot of variation in how to approach ACL ruptures. We use the most advanced techniques here and continually evaluate how they might be refined to improve outcomes.”
- Grimm PD, Mauntel TC, Potter BK. Combat and Noncombat Musculoskeletal Injuries in the US Military. Sports Med Arthrosc Rev. 2019 Sep;27(3):84-91.
- Zaid MB, OʼDonnell RJ, Potter BK, Forsberg JA. Orthopaedic Osseointegration: State of the Art. J Am Acad Orthop Surg. 2019 Nov 15;27(22):e977-e985.
- Valerio IL, Dumanian GA, Jordan SW, Mioton LM, Bowen JB, West JM, Porter K, Ko JH, Souza JM, Potter BK. Preemptive Treatment of Phantom and Residual Limb Pain with Targeted Muscle Reinnervation at the Time of Major Limb Amputation. J Am Coll Surg. 2019 Mar;228(3):217-226.
