Inhaled Steroids a Factor
Veterans with COPD have been hit hard by an increase in nontuberculous mycobacteria infections. Researchers suggest that treatment with inhaled steroids appears to play a role in the rising rates, but many other factors also are involved. The key, according to VA clinicians, is to make sure that inhaled steroids are used only in patients who benefit most.
MIAMI—Among veterans with chronic obstructive pulmonary disorder, the rate of nontuberculous mycobacteria infections have risen sharply since 2001, and treatment with inhaled corticosteroids appears to have substantially increased the risk.
A study by researchers at the Miami VA Healthcare System also cautioned that NTM can significantly increase mortality risk in patients who develop it.1
While not contagious, NTM infection can be fatal. Treatment can require up to two years of expensive antibiotic therapy, as a growing number of NTM species have developed resistance to many common antibiotics.
Nontuberculous mycobacteria include more than 150 types of bacteria that commonly occur in soil and water. Some individuals appear particularly susceptible to pulmonary infections with the gram positive, acid-fast organisms, particularly those with suppressed immune systems, bronchiectasis, COPD or lung damage. Tall, slim white women also have greater risk, as do the elderly and individuals with acid reflux, according to the American Lung Association.
Several studies have documented rapidly rising rates of nontuberculous mycobacteria infections globally. In the United States, studies show prevalence per 100,000 increased from 1.8 to close to 40 since the 1980s.
The VA researchers found that the incidence of NTM in veterans with COPD doubled between 2012 and 2015, while the prevalence tripled over a 15-year period, with a sharp uptick after 2012.
Multiple Factors
“Veterans with COPD have an increased risk for NTM,” explained co-author Mehdi Mirsaeidi, MD, MPH, of the pulmonary medicine section of the Miami VA and an assistant professor the University of Miami Miller School of Medicine. “Corticosteroids used for treatment increases risk 2.5 times, according to a study in California.”
That study, published in the Annals of the American Thoracic Society, found that the longer a person took inhaled corticosteroids and the higher the dose, the greater the risk of an NTM infection.2
While clearly beneficial in patients with asthma, the use of the drugs in COPD has come into question, said Stephen J. Ruoss, MD, senior study author and a pulmonologist and intensivist at Stanford University Medical Center in California. Recent guidelines recommend physicians prescribe them only to patients with COPD who experience frequent exacerbations.
“There have been some big studies that have shown a very modest, but statistically significant benefit of inhaled steroid use in COPD patients,” Ruoss said, adding that studies also demonstrate that COPD patients who use ICS have a greater risk of bacterial infections. “As physicians, we should be careful using this class of drugs broadly in patients with COPD.”
“There is an association between ICS and NTM,” Mirsaeidi told U.S. Medicine, but he cautioned against putting all the blame on the medications or assuming that all patients would be better off without them.
“Inhaled corticosteroids control exacerbations in some patients. If they stop using them, they will have more exacerbations, and that may lead to higher death rates. So, yes, rates of pneumonia and other infections go up with their use, but we must weigh the risk against greater inflammation in the lungs,” he said. “We need to learn more about who is really the best patient for inhaled corticosteroids.”
Other options might include use of a steroid-free medication. Last fall, the Food and Drug Administration approved new labeling for tiotropium bromide and olodaterol inhalation spray, marketed as Stiolto Respimat. Data showed meaningful reduction in COPD exacerbations driven by tiotropium.
The FDA also revised the indication for Stiolto Respimat, which is now approved for the treatment of patients with COPD, including chronic bronchitis and emphysema. Previously, the inhalation spray was approved for the treatment of airflow limitation in patients with COPD, including chronic bronchitis and emphysema.
Factors other than medication therapy play a significant role in the increased risk of infection in patients with COPD, Mirsaeidi added. “Many studies show that patients with COPD have concurrent bronchiectasis. Chronic inflammation, COPD and bronchiectasis can all change the immune system.”
Those changes make veterans with these lung diseases more susceptible to infections generally. “The overall immune system of COPD patients does not work like other patients. The T-cells do not function as well. The chronic inflammation changes the CD8 and CD4 cells. Their immune systems do no interact with microphages in a normal way,” he noted.
Presenting Like TB
NTM lung disease can present much like tuberculosis with a persistent cough, coughing up blood, shortness of breath, fatigue, low grade fever, night sweats and unexplained weight loss. The two diseases can look so similar that up to 30% of patients with treatment-resistant tuberculosis actually had NTM instead, according to a study by Mirseidi.3
In other instances, NTM may cause lung disease with nonspecific symptoms that may resemble other pulmonary disorders including COPD, cystic fibrosis or bronchiectasis.
“”The increasing prevalence of NTMs is disconcerting because some of the most common types of NTM are harder to treat than multidrug-resistant TB,” Ruoss said.
The VA researchers analyzed records of more than two million COPD patients at VA hospitals between 2001 and 2015 to better understand the rate of NTM infection and the impact of the infection on mortality in this vulnerable population. The study appeared in Frontiers of Medicine.
Among veterans with COPD, the incidence rate per 100,000 stayed stable at about 34 for the years 2001 to 2012, before rocketing to 70.3 in 2015. Prevalence rates per 100,000 tripled over the same time period, rising from 93.1 in 2001 to 277.6 in 2015, with a particularly sharp increase after 2012.
The infections proved far from benign. The researchers found NTM infections increased mortality risk 43% among veterans with COPD compared to uninfected veterans with COPD.
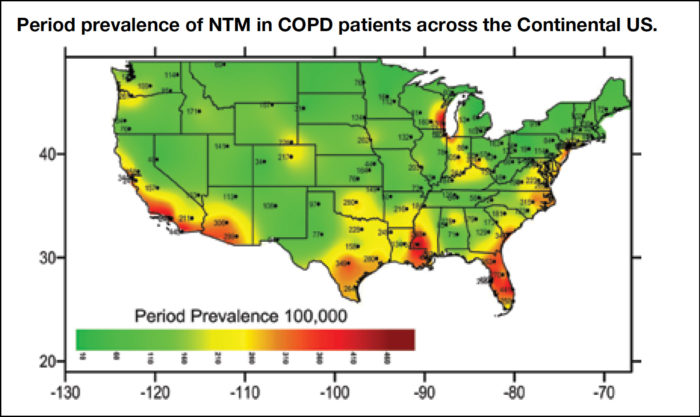
The study also documented a significant variance in rates of infection based on geography, with rates of nontuberculous mycobacteria infection among veterans with COPD nearly 10 times higher in some states than in others. Puerto Rico, Florida and Washington, DC, had more than 309 to 370 cases per 100,000, while South Dakota, Montana and Missouri had between 31 and 75 cases per 100,000. Most of the nation’s clusters of infection occurred around lakes and the coasts.
Environmental factors largely drive the differences in prevalence. “Moisture, lower pH of the water and soil, warmer temperature, all increase the risk of NTM. The climate in Florida and Puerto Rico is very similar and the soil in DC has a pH of 6.2 to 6.3, which is good for its growth, too,” said Mirsaeidi. “West Texas has a pH of 7.0 to 7.6, which is good for other mycobacteria.”
1 Pyarali FF, Schweitzer M, Bagley V, Salamo O, Guerrero A, Sharifi A, Campos M, Quartin A, Mirsaeidi M. Increasing Non-tuberculous Mycobacteria Infections in Veterans With COPD and Association With Increased Risk of Mortality. Front Med (Lausanne). 2018 Nov 6;5:311.
2 Liu VX, Winthrop KL, Lu Y, Sharifi H, Nasiri HU, Ruoss SJ. Association between Inhaled Corticosteroid Use and Pulmonary Nontuberculous Mycobacterial Infection. Ann Am Thorac Soc. 2018 Oct;15(10):1169-1176.
3 Mirsaeidi M, Machado RF, Garcia JGN, Schraufnagel DE. Nontuberculous Mycobacterial Disease Mortality in the United States, 1999–2010: A Population-Based Comparative Study. PLoS ONE, 2014; 9 (3): e91879 DOI: 10.1371/journal.pone.0091879
