Discontinuation of sodium-glucose co-transporter-2 (SGLT2) inhibitors and glucagon-like peptide-1 receptor agonists (GLP-1 RA) is common but is associated with harmful outcomes in adults with chronic kidney disease (CKD), according to a recent study.
Early Dialysis Leads to Modest Gains in Life Expectancy, Less Home Time
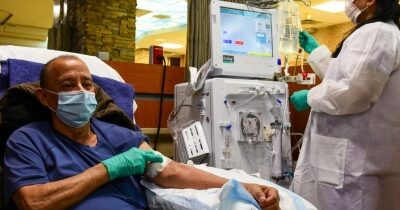
Older adults with reduced kidney function who start dialysis within 30 days and aren’t referred for transplant have modest gains in life expectancy and less time at home, according to a recent study.
Microvascular Complications of Type 2 Diabetes Drop When PTSD Resolves in Veterans
Post-traumatic stress disorder (PTSD) has a range of adverse effects in veterans, and about 7% are affected at some point in their lifetimes. A recent study puts a spotlight on an unexpected co-morbidity—worsening Type 2 diabetes (T2D) outcomes.
Study: Eating Processed, Red Meat Raises the Risk of Type 2 Diabetes
Consuming meat, especially processed and red meat, is a risk factor for the development of type 2 diabetes, according to a new study involving VA researchers.
Revised Guidelines Give Recommendations Concerning Use of Newer Pharmacological Treatments for Type 2 Diabetes
The newest medications for Type 2 diabetes have benefits beyond controlling blood sugar. Evidence suggests they also reduce mortality and the risk of cardiac events.
Gout Largely Treatable, but a Considerable Burden in Older Veterans
One of the earliest recorded and most intensely painful diseases, gout was historically called the “disease of kings.” For centuries, it was thought to affect only the wealthy and aristocratic.
VA Clinicians Tackle Issue of Defining and Combatting ‘Diabetes Distress’
The term “diabetes distress” is used to describe the emotional response to living with diabetes, a life-threatening illness that requires chronic and demanding self-management.
Study Emphasizes Importance of β-cell Function Loss in T2D Progression
For the estimated 1 in 10 Americans—or 1 in 4 veterans—with Type 2 diabetes, keeping blood glucose levels in the near-normal range reduces the risk of complications such as heart, kidney and eye disease.
Diabetic CKD Progression Faster in Veterans Than General Population
Veterans with diabetic kidney disease have a faster rate of stage progression compared to patients in the general population, and more than half of veteran diabetic kidney disease patients progressed to an advanced stage or died within 5 years, according to a recent study.
New Study Defines Clinically Important Measures of Diabetes Distress
The term “diabetes distress” is used to describe the emotional response to living with diabetes, a life-threatening illness that requires chronic and demanding self-management.
Cardioprotective Drugs Not Also Used in Patients Needing Them Most
Even though the overall uptake of cardioprotective antihyperglycemic drugs has increased as second-line treatments for Type 2 diabetes mellitus, over the last decade, patients who actually have cardiovascular disease were less likely to be prescribed them compared to those without CVD.
Strict LDL-C Lowering Linked to Diabetes Progression
While some guidelines recommend statin use to achieve low-density lipoprotein cholesterol (LDL-C) goal under 70 mg/dL for primary prevention of atherosclerotic cardiovascular disease (ASCVD) in patients at higher risk, others recommend against a target LDL-C level.
Glycemic Control Not Affected Much By Neighborhood Factors
How do demographic, social and geographic factors affect glycemic control over time in veterans newly diagnosed with diabetes?
Diabetes Has Surprising Effect on Prostate Cancer Prognosis
How diabetes affects the prognosis of advanced prostate cancer (PC) is not well documented, according to a new study which sought to provide more information.
Statins Play a Role in Type 2 Diabetes Progression to Insulin Use
In patients with Type 2 diabetes mellitus, cardiorespiratory fitness and body mass index (BMI) play a role in statin-related progression to insulin therapy, according to a recent study.
Anti-VEGF Injections Can Cause Adverse Events in Veterans With Diabetes
Diabetes patients who are treated with anti-vascular endothelial growth factor (VEGF) injections, the primary treatment for diabetic retinopathy, have a higher likelihood of experiencing adverse events, such as acute myocardial infarction, cardiovascular disease or kidney disease, according to a recent study.
Which T2D Drug Class Prevents CVD Best in Patients Without Previous Disease?
In 2020, in its annual revision of the Standards of Medical Care in Diabetes, the American Diabetes Association (ADA) made some significant changes in recommendations.
Adherence to Diabetes Medications Remained High During COVID-19 Pandemic
During the COVID-19 pandemic, high-risk diabetes patients who were treated in the VA Healthcare System adhered to their diabetes medication regimens and maintained high primary care use, even though virtual care replaced in-person care, according to a recent study.
GLP-1 RAs, Other Agents, Underused in Patients Who Need Them the Most
While news reports focus on high demand for glucagon-like peptide-1 receptor agonists (GLP-1 RA), the real story might be widespread under use of those agents and others that reduce the risk of cardiovascular disease and chronic kidney disease progression in patients with Type 2 diabetes.
Weight Loss Similar in Older/Younger Veterans on Semaglutide
Concerns have been raised about GLP-1 receptor agonists causing unintended weight loss in older adults. A new VA study has put that worry to rest, finding no significant difference in weight loss with semaglutide use among veterans 65 or older compared to those who are younger. The authors concluded that age does not appear to be a “robust predictor” of semaglutide’s effect on weight.
Cardiorespiratory Fitness Linked to Lower Abnormal Glucose Risk
Cardiorespiratory fitness (CRF) can be a good predictor of chronic disease. The problem is the difficulty and impracticability of routinely measuring that in primary care settings.
Cardiac Autonomic Neuropathy Linked to Stroke in T2D
What is the association between cardiac autonomic neuropathy (CAN) with incident stroke among diabetes mellitus patients?
Time in Range Beneficial in Patients With Individualized A1c
Individualizing hemoglobin A1c treatment goals in older adults is important to balance risks in benefits, according to a new study.
Elevated Preoperative Glucose Level Linked to Adverse Effects in Hernia Repair
An estimated 1 in 10 Americans and 1 in 4 veterans has diabetes, not only putting them at increased risk for problems such as heart and kidney disease, but also making them more prone to complications such as infection and bleeding following surgery.
Diabetes Drug Metformin Shows Promise for Reducing Incident Osteoarthritis
Metformin is recommended as first-line therapy for Type 2 diabetes at the VA and elsewhere. Among the benefits, according to the VA PBM, is that the drug, which has been in use for decades, is low-cost and safe to initiate in most patients, even those with moderate renal dysfunction.
Dietician Mary Julius Champions VA’s Virtual Diabetes Education Program
When Mary Julius was diagnosed with Type 1 diabetes in 1974, the world was a very different place. There were only approximately 4.5 million Americans who had been diagnosed with diabetes.
Overall Prescriptions Are Low at VHA for CVD, CKD Protective Diabetes Drugs
Even though novel therapies for type 2 diabetes have been proven to reduce the risk of cardiovascular disease and chronic kidney disease progression, VHA prescription rates remain low.
Glargine, Liraglutide More Effective for Reaching, Maintaining T2D Targets
Clinicians treating Type 2 diabetes have an arsenal of medications to help lower glucose levels in patients with uncontrolled blood sugar. The key question regards which work best to lower glucose levels and keep them low.
Diabetes Genetic Risk Score Linked to Dementia in Some Veterans
Using the VA’s Million Veteran Program data, a new study has determined that a diabetes genetic risk score is associated with all-cause dementia and clinically diagnosed vascular dementia in veterans.
Rural T2D Patients Improved With Remote VA Care
How did a novel approach to provide diabetes specialty team care to rural veterans with Type 2 diabetes (T2DM) affect clinical outcomes and processes of care?