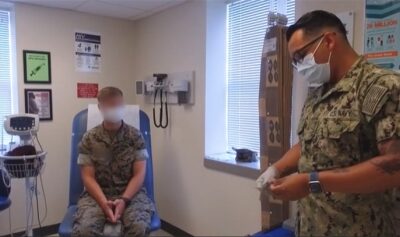
Consistent use of HIV preexposure prophylaxis (PrEP) has been shown to reduce the risk of sexual risk of HIV acquisition by 99% among men who have sex with men (MSM).
VA Study: Microbial Contamination Continues in Hospitals, Even When Recommended Cleaning Protocols Are Followed
Microbial contamination—including pathogenic and potentially pathogenic bacteria—persisted on high-touch hospital surfaces despite compliance with recommended disinfection protocols, according to a study performed at the Central Texas Veterans Healthcare System.
COVID-19 Mortality Looks Somewhat Different Based on New VA Study
A study team involving VA researchers looked at death rates during the COVID-19 pandemic through a different lens and came up with intriguing information from individual-level instead of aggregate data.
Military/VA Study Finds That Smallpox Vaccination Is Effective Against MPox
The smallpox vaccine appeared to be effective in preventing mpox (formerly called monkeypox) in U.S. military personnel and veterans, even if received more than a decade previously, according to a new report.
Too Few VA Anal Cancer Exams in HIV Patients
Because human immunodeficiency virus (HIV) patients are at high risk for anal cancer, screenings are recommended annually for U.S. veterans with HIV.
Flexible Prevention Bundle Appears to Reduce Some Surgical Site Infections
Surgical site infections (SSIs) are associated with significant morbidity and mortality, prolonged length of hospital stay and readmission.
Lower Risks of Adverse Effects in Older Adults With Moderna COVID-19 Vaccine
Receipt of the Moderna COVID-19 vaccine by older adults was associated with a lower risk of adverse events than the Pfizer-BioNTech version, according to a new study.
Antibiotic Prescribing High for Respiratory Infection Patients; HIV Not a Factor
Inappropriate antibiotic prescribing for acute respiratory infections, a major public health concern, is high in both patients with and without human immunodeficiency virus (HIV) and doesn’t appear to be affected by HIV status, according to a recent study.
VA Doctor-Turned-Inventor Works to Prevent Infectious Disease Spread
Part of the inspiration for Chetan Jinadatha, MD, MPH, to specialize in treating infectious disease comes from going to medical school in his native India, which has a high burden of such diseases. However, he also likes to say it’s partly for selfish reasons.
VA Researchers Find Biomarkers for Potentially Serious Parasitic Infections
Asymptomatic Leishmaniasis Infected Nearly 20% of Soldiers in Iraq BETHESDA, MD—New research has identified three chemokines as potential biomarkers for asymptomatic visceral leishmaniasis (VL), a chronic infection caused by Leishmania (L.) donovani or L. infantum....
Do Fungal Pathogens Cause ARI More Often Than Previously Suspected?
Fungal infections are known to be causes of community-acquired pneumonia (CAP) and acute respiratory illness (ARI), but it is not clear how their frequency compares with that of viral and bacterial causes of these conditions.
Paxlovid Reduces Likelihood of Long COVID in Patients at Severe Infection Risk
A recent study suggested, that Paxlovid, which is prescribed to patients infected with SARS-CoV-2, who are at risk for severe symptoms, also might help protect against the condition. Researchers found the antiviral also lowered the likelihood of post-acute death and hospitalization.
VA Spent Millions on HPV-Related Cancer But No Vaccination Promotion
Vaccinations for Veterans, Servicemembers Half of Civilian Rate ST. LOUIS—Eligible active-duty servicemembers and veterans have dramatically lower rates of human papillomavirus (HPV) vaccination, placing them at much greater risk of related cancers, according to a new...
HIV Patients Have Worse Long-Term Survival Following Coronary Procedure
The burden of cardiovascular disease among HIV patients has tripled over the past few decades, and cardiovascular mortality has steadily risen.
Survey Examines COVID-19 Vaccination Hesitancy Among U.S. Soldiers
Soldiers who agree with COVID-19 vaccination effectiveness, safety or importance, as well as soldiers who have an immediate supervisor who encourages them to get the COVID-19 vaccine, are more likely to get vaccinated, according to a new study.
What About Servicemembers Discharged for COVID-19 Vaccine Refusal?
DoD officially rescinded the COVID-19 vaccine mandate for servicemembers last month. Even though President Joe Biden and DoD leaders opposed the move
Study Examines Reasons for Vaccine Hesitancy in Patients With IBD
Even after years of the COVID-19 pandemic, data remains somewhat limited on the safety profile of SARS-CoV-2 vaccine in patients taking immunosuppressive medications.
COVID-19 Reinfection Adds Significant Risk to Multiple Organ Systems
Despite misconceptions that prior COVID-19 infections can keep patients from having severe cases in the future, a new study suggests that recurrent cases pile on the risk of adverse health conditions in multiple organ systems.
Factors Linked to Severe COVID-19 Among Vaccinated, Hospitalized Veterans
Although vaccination and boosting remain the best defense against COVID-19, breakthrough infections among those vaccinated and boosted are exceedingly common.
Polypharmacy Associated With Worse Outcomes in Veterans With HIV
The good news, according to a recent study, is that medical intensive care unit (MICU) admissions have been declining in people with HIV infection (PWH).
Degree of Diastolic Dysfunction Similar With and Without HIV
Human immunodeficiency virus (HIV) infection is known to be associated with subclinical cardiomyopathy, diastolic dysfunction and increased risk of cardiovascular death.
HIV Prevention Use Remains Too Low in U.S. Military
Even though about 20.9% of U.S. servicemembers report a high risk of HIV infection, only about 2,000 of them had accessed HIV pre-exposure prophylaxis (PrEP), as of 2017.
Severe COVID-19 Illness Low for Veterans After Vaccination Plus Booster
Veteran patients who received a COVID-19 vaccination series, plus a booster vaccine dose, had a low incidence of hospitalization, death or severe illness from COVID-19, according to a new study.
DHA: Chlamydia Is the Most Common Sexually Transmitted Infection Among Active Duty U.S. Military Servicemembers
Chlamydia is the U.S. military’s most common sexually transmitted infection (STI) among active duty servicemembers, according to 2021 and 2022 reports on STIs by the Defense Health Agency’s Armed Forces Health Surveillance Division.
VA Receives First Doses of Vaccine to Help Combat Monkeypox Outbreak
When the World Health Organization declared monkeypox a public health emergency on July 23, there were more than 4,000 reported cases in the United States. By mid-September, the number of reported U.S. cases had surpassed 24,000.
Clostridioides Difficile Infection Increases Mortality, Costs for MHS Patients
One of the largest studies ever of healthcare-facility-associated Clostridioides difficile infection (CDI) underscored the seriousness of the infection, which causes significantly increased length of stay, higher costs, and, worst of all, greater mortality among inpatients.
Blood Sugars Higher for Flu Vaccine Recipients With Diabetes
The Vaccine Adverse Effect Reporting System, established by the national Centers for Disease Control and Prevention, has more than 350 reports of hyperglycemia post-influenza vaccine, according to a new study.
Elderly Veterans More Likely to Die from COVID-19 Than Flu
An often repeated misconception during the COVID-19 pandemic is that the Sars-C0V-2 and influenza viruses are similarly fatal for older adults, although there have been limited data to support that observation.
Yellow Fever Vaccine Response Lower After Flu Vaccine
The DoD’s support of the United States government’s response to the Ebola crisis in Liberia, beginning in 2014‐2015, was the first U.S. military operation to support a disease‐driven foreign humanitarian assistance mission.
Clonal Hematopoiesis Does Not Predict Severe COVID-19
COVID-19 cases range dramatically from severity, from asymptomatic to self-limited influenza-like illness to severe respiratory failure or even death.