As many as 40% of breast cancer survivors are dissatisfied after breast reconstruction due to unexpected outcomes that don’t meet personal preferences.
Internal VA Investigation Verified Sexual Harassment Complaints Within ORMDI
An internal VA investigation has verified many, though not all, of the sexual harassment allegations made public by members of the House VA Committee in January.
Rare Congressional Subpoena for VA in Sexual Harassment Investigation
The House VA Committee has voted to subpoena VA Secretary Denis McDonough to release documents pursuant to an ongoing sexual harassment investigation involving several supervisors in VA’s Office of Resolution Management, Diversity, and Inclusion.
Women Veterans With Epilepsy Have More Psychiatric Diagnoses
Women Veterans with epilepsy (WVE) might have unique psychiatric comorbidities that affect presentation, treatment and outcomes.
Cardiac Mortality for Women Veterans Has Not Improved Over Two Decades,
Women veterans have shown a lack of improvement in cardiac mortality compared to civilian women over nearly two decades, suggesting a need for clinical interventions to improve cardiovascular care, according to a recent study.
Pregnant Veterans Often Discontinue Antidepressants, Monitoring Needed
VA medical providers and veterans need more education about the risks and benefits from continuing antidepressants during pregnancy, according to a new study.
Uterine Cancer Mortality Increased Sharply in Some Groups
Since the beginning of the 21st century, uterine cancer mortality has increased, especially among Black and Hispanic women, according to a new study.
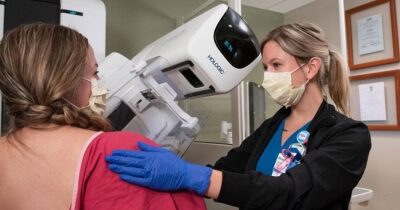
Military Health Mammography Lapses During Pandemic Spotlights Disparities
Breast cancer screening within the Military Health System (MHS) plummeted by 74% in the early COVID-19 pandemic period and 22% in the late pandemic period, compared with the prepandemic period.
Army Files Charges Against Anesthesiologist, Alleges Inappropriate Sexual Conduct
Sexual-assault charges have been filed by the Army against Maj. Michael Stockin, MD, an anesthesiologist stationed at the pain clinic at Joint Base Lewis-McChord’s Madigan Army Medical Center.
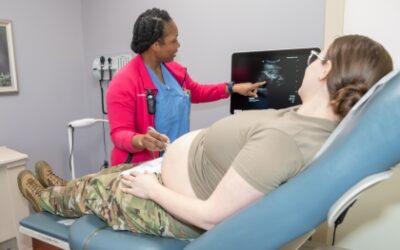
VA Expands Program Caring for Pregnant Veterans, New Mothers
As of this month, mothers treated by the VA healthcare system pre- and post-partum have access to maternity care coordinators from the beginning of their pregnancy to 12 months after birth. That is a change from the previous end-date of 8 weeks post-partum.
Women Serving in Gulf War Demonstrated Worse Health Outcomes Than Others
Women veterans who deployed to the 1990-1991 Gulf War report poorer health than Gulf War Era veterans who served during that time but didn’t deploy and women in the U.S. general population, according to a recent study.
Recent Lawsuits Challenge In Vitro Fertilization Policies at VA, DoD
A lawsuit filed recently in federal court in Manhattan challenges the eligibility policies of DoD and VA for who can receive in vitro fertilization (IVF) care, calling them discriminatory.
VA Is Screening for Breast Cancer in Veterans Under 40 With Toxic Exposures
Veterans younger than age 40 might be eligible for breast cancer risk assessments and mammograms if they were exposed to burn pits and other toxins during their service, according to the VA.
Racial Disparities Persist in Outcomes for Pregnant and Postpartum Veterans, as Well as Their Infants, Despite VA’s Equal Access System
Racial health disparities in the United States are well documented, but the starkest are with reproductive health and outcomes, according to a VA researcher.
Survival Rates Trend Lower in Non-Hispanic Black Patients With Uterine Cancer
Disparities in survival exist between non-Hispanic Black and non-Hispanic white patients with uterine cancer. A new study from military researchers sought to determine why.
VA Study Shows Low Use of Primary Care for Reproductive Health Services
The integration of reproductive health services into primary care practices is increasingly recognized as critical to the advancement of patient-centered care and improving reproductive outcomes.
Quality Care Reduces Breast Cancer Survival Rate Disparities Based on Race
Though non-Hispanic Black women are more likely to have tumors at a higher grade and later stage and be diagnosed with triple-negative breast cancer
Promotion Delays Affecting Military Readiness But Senator Won’t Budge
Delays in promotions directly impacts military readiness, DoD officials have said. But there isn’t much they can do about it as long as Sen. Tommy Tuberville (R-AL) is blocking the expedited promotion of more than 150 military generals and flag officers
Republicans Seek to Overturn VA Policy to Provide Abortion Services
Republicans in the House and Senate have reintroduced a resolution to reverse VA’s recent policy change that allows for limited abortion counseling and services at its facilities.
VA Spent Millions on HPV-Related Cancer But No Vaccination Promotion
Vaccinations for Veterans, Servicemembers Half of Civilian Rate ST. LOUIS—Eligible active-duty servicemembers and veterans have dramatically lower rates of human papillomavirus (HPV) vaccination, placing them at much greater risk of related cancers, according to a new...
VA Employee Sues Over VA’s Decision to Provide Abortion Services
When VA announced in September that it would be allowing department clinicians to provide abortions and abortion counseling in response to the overturning of Roe v. Wade, it was widely anticipated that there would be lawsuits from state governments that restrict abortion access.
Intimate Partner Violence More Common With Veterans, Military Personnel
VA should be doing more to identify and support victims of intimate partner violence (IPV), according to a recent VA Office of the Inspector General (OIG) report that also maintained that programs already in place are inconsistently implemented.
Republican Legislators Express Strong Opposition to VA Offering Abortion Services
VA officials believe that the overturning of Roe v. Wade in June and the subsequent enforcement of abortion bans in several states creates a clear danger to the health of women veterans.
DHA: Chlamydia Is the Most Common Sexually Transmitted Infection Among Active Duty U.S. Military Servicemembers
Chlamydia is the U.S. military’s most common sexually transmitted infection (STI) among active duty servicemembers, according to 2021 and 2022 reports on STIs by the Defense Health Agency’s Armed Forces Health Surveillance Division.
VA Adds Abortion Counseling, Limited Abortion Access to Health Services
The VA has expanded its health services to include access to abortion counseling and, in limited cases, abortion to veterans and VA beneficiaries, even when restricted by state laws.
Sexual Harassment Reporting Structure Might Change at VA
Despite concerns from agency watchdogs that VA’s sexual harassment reporting process has a perceived conflict of interest, if not an actual one, the department has resisted changing it.
VA OIG: Lack of Oversight Found in DO’s Sexual Abuse at Beckley VAMC
This is just the latest finding by the OIG that places blame for a recent criminal case on lack of VA oversight.
Arkansas VAMC Illuminates Bladder Cancer Using Blue Light Cystoscopy
Early-stage cancers can be very challenging to see, but finding them before they advance provides the best chance for curative treatment with the fewest complications.
The Role of Social Determinants in Cancer in Young Women
Oncology research continues to better understand and quantify the role that social determinants play in the development of cancers to help find ways to reduce the burden of cancer on society and individuals.
Women with Pathogenic Variants Excluded from Germline Testing after DCIS
Every year, 60,000 women in the United States receive a diagnosis of ductal carcinoma in situ (DCIS), a noninvasive form of breast cancer. Accounting for one in five breast cancer diagnoses, DCIS has increased with the adoption of routine mammography, but it is far more than just an artifact of imaging.