Veterans who experience housing instability have an elevated risk of developing Alzheimer’s disease or a related dementia compared to those with stable housing, according to a recent study.
New Therapies Have Improved Survival for Prostate Cancer Patients
Improved treatment has meant better overall survival for many men diagnosed with prostate cancer, according to a new research letter. For older patients, however, the benefits of the new therapies weren’t as effective, the authors pointed out.
GOP Lawmakers Challenge Data That COVID-19 Vaccine Protected Troops
Recent data from DoD seems to confirm what researchers and physicians have been saying for years—that individuals who receive the COVID-19 vaccine are less likely to experience long-term health effects than those who do not.
HCC Tumor Recurrence After Radiologic Responses
How often does local recurrence occur in hepatocellular carcinoma (HCC) patients who undergo selective transarterial radioembolisation (TARE) or transarterial chemoembolisation (TACE) and achieve a complete response (CR) radiologically?
Biomarkers Help Predict Which Cirrhosis Patients Develop HCC
It can be difficult to determine which patients with cirrhosis will go on to develop hepatocellular carcinoma (HCC).
Accelerated PACT Timeline Opens VA Healthcare to Many More Veterans
VA has dramatically accelerated the healthcare provision of the PACT Act, opening healthcare enrollment to hundreds of thousands of veterans who might have been exposed to toxic substances during their service.
Misclassification Affects Estimates of Opioid-Use Disorder Medications
Is misclassification of people who inject drugs (PWID) and are hospitalized because of infections affecting the analysis of outcomes from medications for opioid-use disorder (MOUD?
Study: Racism Contributes to Low OUD Prescribing in MHS
Rates of prescribing for medication for opioid-use disorder (MOUD) are low in the MHS and show evidence of institutional racism, according to a new study.
Long-Acting Benzodiazepines Best for Alcohol Withdrawal in Veterans
An extensive study of VA patients concluded that the best way to manage alcohol withdrawal in hospitalized settings is the use of long-acting benzodiazepines with symptom-triggered therapy, as recommended in American Society of Addiction Medicine (ASAM) guidelines.
Does ‘Underserved’ Designation Demoralize Staff at VA Facilities?
For the past several years, VA has been identifying the most underserved facilities in its system and requiring them to create action plans to improve care to their veterans.
VA Telemedicine Rates Remain High After COVID-19 Pandemic, Especially for Mental Healthcare Visits
Following the COVID-19 pandemic, telemedicine rates for veterans enrolled in VA healthcare services remained high, accounting for more than half of mental healthcare visits, while telephone-based care has decreased to pre-pandemic levels, according to a recent study.
Psychoactive Drug Ibogaine Effectively Treats TBI Complications
The signature injury of U.S. veterans from recent military conflicts, traumatic brain injury (TBI) is a leading cause of injury-related disability.
Internal VA Investigation Verified Sexual Harassment Complaints Within ORMDI
An internal VA investigation has verified many, though not all, of the sexual harassment allegations made public by members of the House VA Committee in January.
Rare Congressional Subpoena for VA in Sexual Harassment Investigation
The House VA Committee has voted to subpoena VA Secretary Denis McDonough to release documents pursuant to an ongoing sexual harassment investigation involving several supervisors in VA’s Office of Resolution Management, Diversity, and Inclusion.
Opposing Trends for Accidental Death Rates in Returning Soldiers
A longitudinal cohort study, published in the Annals of Epidemiology, determined if risk for accidental death overall, or the most common types of accidental deaths, varied over time in relation to when a soldier returned from a combat deployment.
More Research Needed on High Melanoma Rates in AI/AN People
Non-Hispanic American Indian/ Alaskan Native (AI/AN) people have the second-highest rate of melanoma in the United States after non-Hispanic white people.
Cause of Kidney Injury After Procedures Not Always Contrast Media
The administration of iodinated contrast media is not responsible for all changes in creatinine levels in patients undergoing the procedures.
Black Veterans Get CKD Younger, Have Lower Death Rates
The younger age of chronic kidney disease (CKD) in Black patients can help explain some of the differences and disparities compared to white patients with CKD, according to a new study.
Much More Dual Testing for CKD Needed Within VHA
A new study that included VA researchers made the case for much more dual testing for chronic kidney disease (CKD) in high-risk patients to improve disease management and patient outcomes.
Processing of ICE Medical Claims by VA Sparks Controversy in Congress
Republican legislators butted heads with VA officials last month over the question of whether department resources were being spent on immigrants who have been placed in the custody of Immigration and Customs Enforcement (ICE).
Issues With Pharmacy Module in VA EHR Could Cause Medication Errors
Ongoing problems with the pharmacy module in VA’s new Oracle electronic health record (EHR) have the potential to lead to medication errors, increasing lawmakers’ concern about plans to expand the new system.
VA Has Low Rates of Preoperative Life-Sustaining Treatment Documentation
Surgery is a significant healthcare event that necessitates timely planning for goals of care (GOC), involving discussions about one’s current values, aspirations and treatment preferences.
Some Veterans With Dementia Might Have Treatable Cirrhosis Brain Effects
Could 1 in 10 veterans diagnosed with dementia actually have reversible cognitive decline caused by advanced liver disease?
Cold, Heat Waves Can Present Extra Danger for COPD Patients
Patients with chronic obstructive pulmonary disease (COPD) are adversely impacted by extreme weather conditions, and the effects vary by gender and ethnic backgrounds.
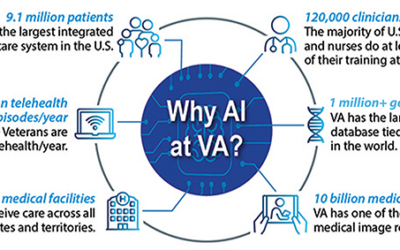
Legislators Told AI Both Promising, Scary for Improving VA Healthcare
The speed at which artificial intelligence (AI) is being embraced at the VA has legislators both hopeful and concerned, optimistic that it can improve veterans’ health but worried about data privacy and the possibility of software superseding human decision-making in clinical settings.
VA Study: Microbial Contamination Continues in Hospitals, Even When Recommended Cleaning Protocols Are Followed
Microbial contamination—including pathogenic and potentially pathogenic bacteria—persisted on high-touch hospital surfaces despite compliance with recommended disinfection protocols, according to a study performed at the Central Texas Veterans Healthcare System.
How Veterans With TBI, GWI Present With Frontotemporal Disorders
Frontotemporal lobe disorders (FTD), which affect personality, behavior and language, are among the most common brain neurodegenerative disorders.
Patient Selection for Lung Cancer Screening Is Less Than Optimal
Clinician judgment, not patient characteristics, often is the deciding factor in which VA patients are screened for lung cancer, according to a new study.
Even Mild COVID-19 Infections Caused Impaired Fitness in Military Personnel
Healthy, young members of the military who have had COVID-19 may experience impairments in fitness up to a year after their acute illness has resolved
White Patients Much More Likely to Receive Knee Arthroplasty In MHS
The U.S. Military Health System is touted as an equal-access medical provider, and scores of studies have demonstrated that few racial inequities exist in the treatment it provides for many conditions.