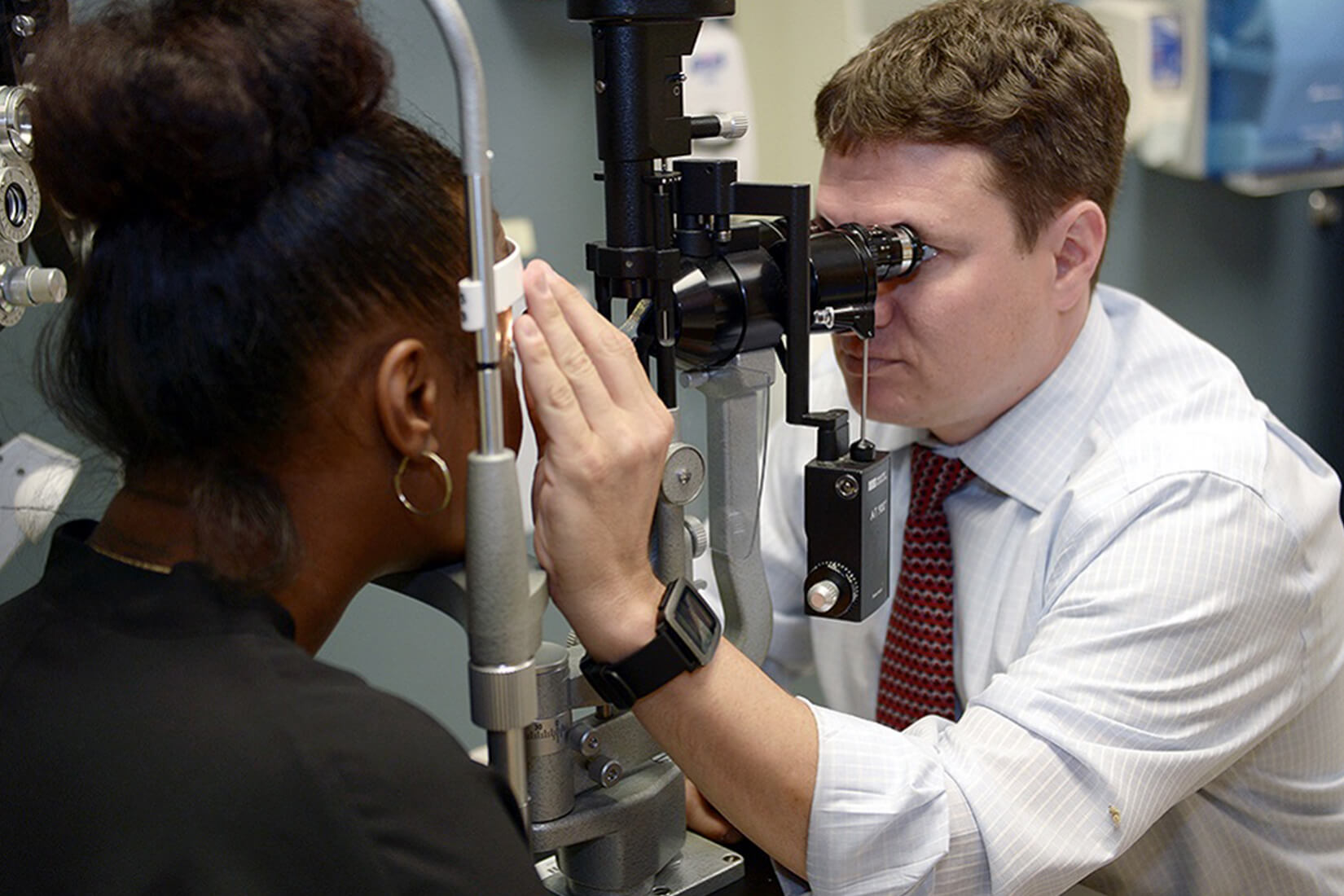
Healthcare System. Regular eye examinations for diabetic patients is one of the areas in which the
healthcare system excels, according to a recent consultant study.
VA photo.
WASHINGTON — The good news from a recent consultant study is that, overall, the VA healthcare system is generally equal or better than others when inpatient and outpatient quality is measured.
The bad news in the RAND Corp. study is the high variation in quality among individual VA facilities.
The study published online by the Journal of General Internal Medicine explained that the VA’s healthcare system was compared to non-VA hospitals for the inpatient comparisons and to commercial HMOs, Medicaid HMOs and Medicare HMOs for the outpatient comparisons.1
“The variation among VA health facilities shows that veterans in some areas are not receiving the same high-quality care that other VA facilities are able to provide,” said co-author Carrie Farmer, a senior policy researcher at RAND.
On the other hand, the variation in the quality of care provided across the VA—which operates the nation’s largest integrated health system—was smaller than what researchers observed among non-VA health providers.
As a whole, the study — which was mandated in the law creating the Choice act, which allows veterans to seek outside care under certain circumstances — found that the VA performed very well. “Consistent with previous studies, our analysis found that the VA healthcare system generally provides care that is higher in quality than what is offered elsewhere in communities across the nation,” emphasized lead study author Rebecca Anhang Price, PhD, a senior policy researcher at RAND, a nonprofit research organization.
Performance Measures
VA’s quality of care in outpatient and inpatient settings was assessed using widely recognized performance measures reported across several national surveys during 2013 and 2014. Among the information analyzed were the Healthcare Effectiveness Data and Information Set and the Survey of Healthcare Experiences of Veterans.
RAND researchers actually compared each of the VA’s 135 facilities to three similar non-VA hospitals based on geographic location and whether the setting was rural or urban. In addition, the healthcare system was measured against other overall care networks.
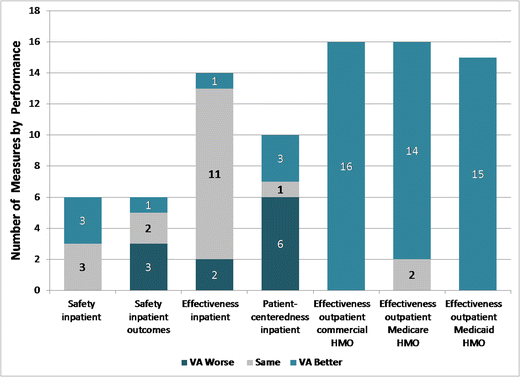
The VA hospitals performed the same or significantly better than non-VA hospitals on:
- all six measures of inpatient safety,
- all three measures of inpatient mortality, and
- 12 measures of the effectiveness of inpatient care.
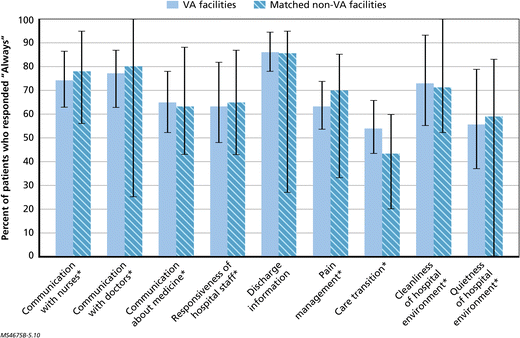
The only areas in which VA hospitals performed significantly worse were three readmission measures and two effectiveness measures. Patients’ experience on pain management was an area where VAMCs scored low, while patient experiences for management of care transitions scored high.
As for the outpatient measures, VA facilities outperformed both commercial HMOs and Medicaid HMOs for all 16 measures of the effectiveness of outpatient care, while doing better than Medicare HMOs on 14 out of 16 measures of effectiveness.
VA care was closest to commercial HMOs in the rate of antidepressant medication management during the acute phase and closest to Medicaid HMOs in the rate of ongoing beta-blocker treatment after an acute heart attack. It far outstripped both of those networks, however, with a high rate of eye examinations for patients with diabetes.
While offering some explanations for the stark differences in care among VAMCs, such as older and sicker patients in some locations, the RAND researchers urged more quality improvement efforts to assure across-the-board excellence in care for veterans.
The VA-funded study pointed out how variable quality ratings were among different facilities in the healthcare system. For example, on the rate of beta blocker treatment for at least six months after discharge for an acute heart attack in 2014, the gap between lowest and highest rated facility was 50 percentage points.
While the study might answer some of the concerns raised by Congress and veterans’ service organizations about quality of care in the VA system, the RAND report did not address access to care or whether it was delivered in a timely manner.
1Anhang Price R, Sloss EM, Cefalu M, Farmer CM, Hussey PS. Comparing Quality of Care in Veterans Affairs and Non-Veterans Affairs Settings. J Gen Intern Med. 2018 Apr 25. doi: 10.1007/s11606-018-4433-7. [Epub ahead of print] PubMed PMID: 29696561.
