Obesity Was Biggest Issue Among Active-Duty Patients
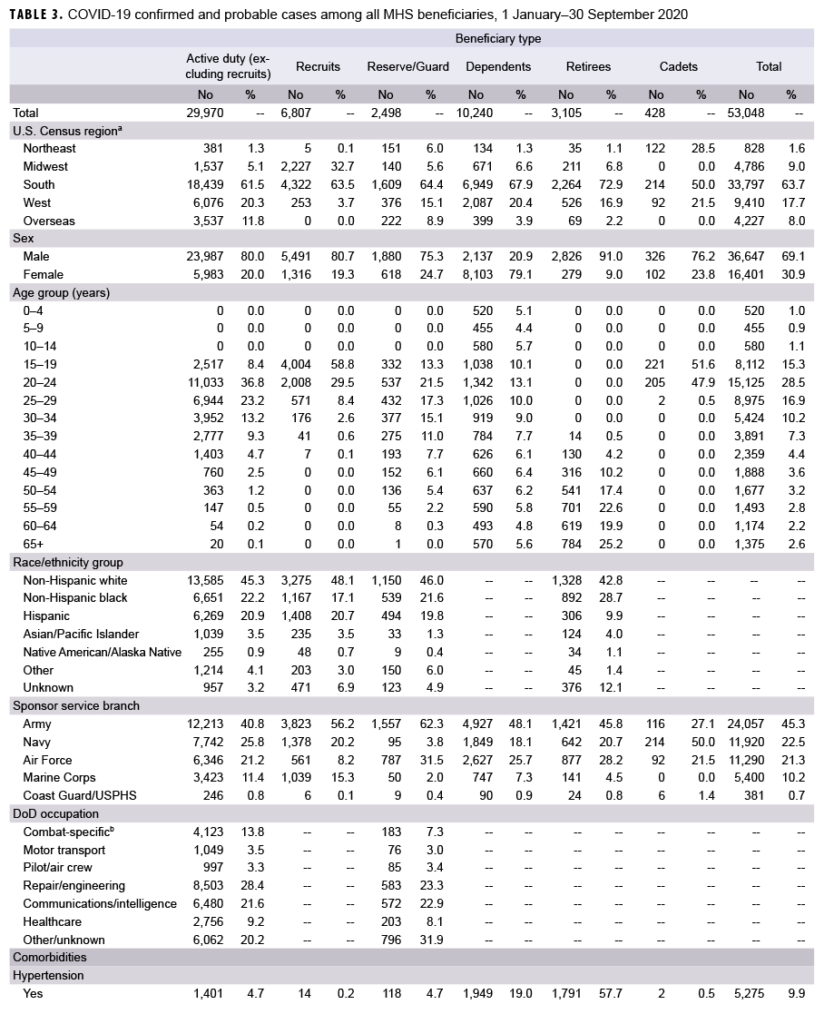
SAN ANTONIO — About a third of COVID-19 cases among MHS beneficiaries were diagnosed with at least one comorbidity linked to more severe infection, and 20% had two or more comorbidities, according to a recent report, which noted that growing rates of obesity likely played a role in the severity of cases in active-duty servicemembers.
The study led by Joint Base San Antonio-Fort Sam Houston, TX, researchers tracked demographic information during the first nine months after COVID-19 was declared a public health emergency. Results indicated that 53,048 MHS beneficiaries were identified as confirmed or probable cases of COVID-19 infection; there were more than 1,800 hospitalizations and 84 deaths.
The authors pointed out that surveillance data of probable and confirmed COVID-19 among MHS beneficiaries have been collected and evaluated on a daily basis since the COVID-19 pandemic began.
“Detailed data on demographic characteristics and underlying medical conditions can inform targeted communication to encourage persons in at-risk groups to practice preventive measures and promptly seek medical care if they become ill,” researchers explained. “Enhanced surveillance efforts can enable actions to prevent and control the current COVID-19 epidemic, which threatens the health of the force.”
The majority of MHS cases were male (69.1%), with 45.4% ages 20-29 years. The demographic and clinical characteristics of these cases varied, however, by beneficiary type—active component service members, recruits, Reserve/Guard, dependents, retirees and cadets.
The article in the MHS’ Medical Surveillance Monthly Report noted that the most common comorbidities present in COVID-19 cases were any cardiovascular diseases (12.7%), obesity or overweight (11.1%), metabolic diseases (10.5%), hypertension (9.9%), neoplasms (7.9%), any lung diseases (7.5%), substance use disorders, including nicotine dependence (5.4%), and asthma (3.2%).1
Early analysis from the national Centers for Disease Control and Prevention (CDC) suggested that patients with underlying health conditions such as chronic obstructive pulmonary disease, cardiovascular disease, diabetes, chronic kidney disease and obesity appeared to be at higher risk for severe COVID-19-associated disease than persons without these conditions. Severe illness from COVID-19 is characterized by a clinical course that results in hospitalization, admission to the intensive care unit (ICU), intubation or mechanical ventilation or death.
Underlying Medical Conditions
Background information in the article pointed out that CDC recently updated its website to include additional underlying medical conditions that might increase one’s risk for severe illness from the virus that causes COVID-19—cancer, chronic kidney disease, COPD (chronic obstructive pulmonary disease), heart conditions such as heart failure, coronary artery disease or cardiomyopathies, immunocompromised state (weakened immune system) from solid organ transplant, obesity (body mass index [BMI] of 30 kg/m2 or higher but < 40 kg/m2), severe obesity (BMI ≥ 40 kg/m2), pregnancy, sickle cell disease, smoking and Type 2 diabetes mellitus.
Here is how cases broke down among different groups covered by MHS:
- Active Duty
As of the end of September, nearly 30,000 active duty servicemembers were detected with the SARSCoV-2 virus infections. The largest demographic proportions of cases were among those who were male (80.0%), aged 20-24 years (36.8%), non-Hispanic White (45.3%) and in the Army (40.8%). Almost one-third (31.7%) of cases were diagnosed with a comorbidity, and 13.5% were diagnosed with two or more comorbidities. Overall, 453 active duty servicemembers (1.5%) were hospitalized, with a median hospital stay of four days (interquartile range [IQR]=3–7); one active-duty servicemember died.
- Recruits
The military identified 6,807 COVID-19 cases among recruits. The largest proportions of cases were male (80.7%), aged 15–19 years (58.8%), non-Hispanic White (48.1%), and in the Army (56.2%). Less than one-tenth (7.6%) of cases were diagnosed with a comorbidity, and only 2.1% were diagnosed with two or more comorbidities. While 89 recruits (1.3%) were hospitalized, with a median hospital stay of five days (IQR=2-7), no deaths occurred among this group during the surveillance period.
- Cadets
By the end of the surveillance period, 428 cadets had been infected with COVID-19 by the end of the surveillance period. Most were male (76.2%) and in the Navy (50.0%). Almost all of the cases were in the 15-19 and 20-24 year age categories (99.5%). Only 3 (0.7%) cadets were hospitalized, and all three cases spent two days in the hospital; none died.
- Reserve/Guard
Reserve and national guard servicemembers had 2,498 confirmed COVID-19 cases during the time period. The largest proportions of cases were male (75.3%), aged 20-24 years (21.5%), non-Hispanic white (46.0%) and in the Army (62.3). Of those, 41 reserve/guard members (1.6%) were hospitalized, with a median hospital stay of four days (IQR=2–7), and seven reserve and guard member died.
- Dependents
With 10,240 dependents identified as COVID-19 cases, the largest proportions of cases were female (79.1%) and dependents of an Army service member (48.1%). There was a wide range in the distribution of age among the dependent cases, but the age categories with the largest numbers of cases were 20-24 years (13.1%), 15-19 years (10.1%) and 25-29 years (10.0%). Of those cases, 590 (5.8%) dependents were hospitalized, with a median hospital stay of four days (IQR=3–8), and 18 died.
- Retirees
Of the 3,105 retirees who were identified as COVID-19 cases, the largest proportions of cases were male (91.0%), non-Hispanic White (42.8%) and formerly in the Army (45.8%). The age categories with the largest numbers of cases were 65 years or older (25.2%), 55-59 years (22.6%), and 60-64 years (19.9%). A much higher percentage, 20, of retiree cases were hospitalized, with a median hospital stay of five days (IQR=3-10). Of the retirees, 58 (1.9%) died of COVID-19 during the surveillance period.
“This report describes the demographic characteristics and prevalence of comorbidities among incident COVID-19 cases across MHS beneficiary categories. Not surprisingly, cases among servicemembers (including recruits and cadets) were most commonly diagnosed in young, non-Hispanic white males, which follows the expected demographic distributions of these groups,” according to the authors.
They pointed out that, among active duty servicemembers, the largest proportion of cases was among Army members (40.8%), which is not unexpected since the Army makes up over one-third of the active component population. Overall, according to the report, 56% of the MHS population that was diagnosed with COVID-19 were active duty members, and 56.5% were between the ages of 20 and 34 years.
Researchers noted that, among servicemember COVID-19 cases, including active duty, reserve/guard, recruits and cadets, obesity/overweight, cardiovascular disease and metabolic disease were among the top comorbidities. They added that, in 2019, the overall prevalence of obesity among active component service members was 17.9% compared to 16.3% in 2015.
“Obesity is relevant to military health because it adversely impacts physical performance and military readiness and is associated with long-term health problems such as hypertension, diabetes, coronary heart disease, stroke, cancer and risk for all-cause mortality,” the authors explained. “The findings presented here further suggest that obesity presents another concern for force health protection in relation to COVID-19, as obesity is one of the most commonly diagnosed comorbidities among active duty member cases.”
- Stidham RA, Stahlman S, Salzar TL. Cases of Coronavirus Disease 2019 and Comorbidities Among Military Health System Beneficiaries, 1 January 2020 through 30 September 2020. MSMR. 2020 Dec;27(12):2-8. PMID: 33393791.