 BOSTON—Many more servicemembers might have been injured by blasts in Iraq and Afghanistan than previously reported.
BOSTON—Many more servicemembers might have been injured by blasts in Iraq and Afghanistan than previously reported.
As of 2017, 380,000 servicemembers had been diagnosed with the signature injury of these conflicts, blast-related traumatic brain injury (TBI), according to the Defense and Veterans Brain Injury Center. Now, it appears that exposure to the explosions might cause physical changes in the brain and cognitive impairment, even in individuals who did not suffer a concussion or mild TBI.
“We were seeing many veterans with concerns about memory and attention,” said Laura Grande, PhD, director of clinical neuropsychology at the VA Boston Healthcare System and an investigator with the VA’s Translational Research Center for TBI and Stress Disorders (TRACTS). “We’d do assessments and find lots of blast exposure, but also PTSD [post-traumatic stress disorder] and substance use.” The complex profile of many patients complicated the determination of what caused the cognitive issues.
Researchers at TRACTS have been able to control for the veterans’ common comorbidities, such as sleep disorders, PTSD and chronic pain, to tease out the impact of blast exposure on brain physiology and function. A study led by Meghan Robinson, PhD, a postdoctoral fellow at TRACTS and the Neuroimaging Research for Veterans Center, found that traditional assessments of blast injury severity based on concussion symptoms fail to capture blast-related neurotrauma in many individuals and could lead to mischaracterization of injury in others.1
Distance From Blast
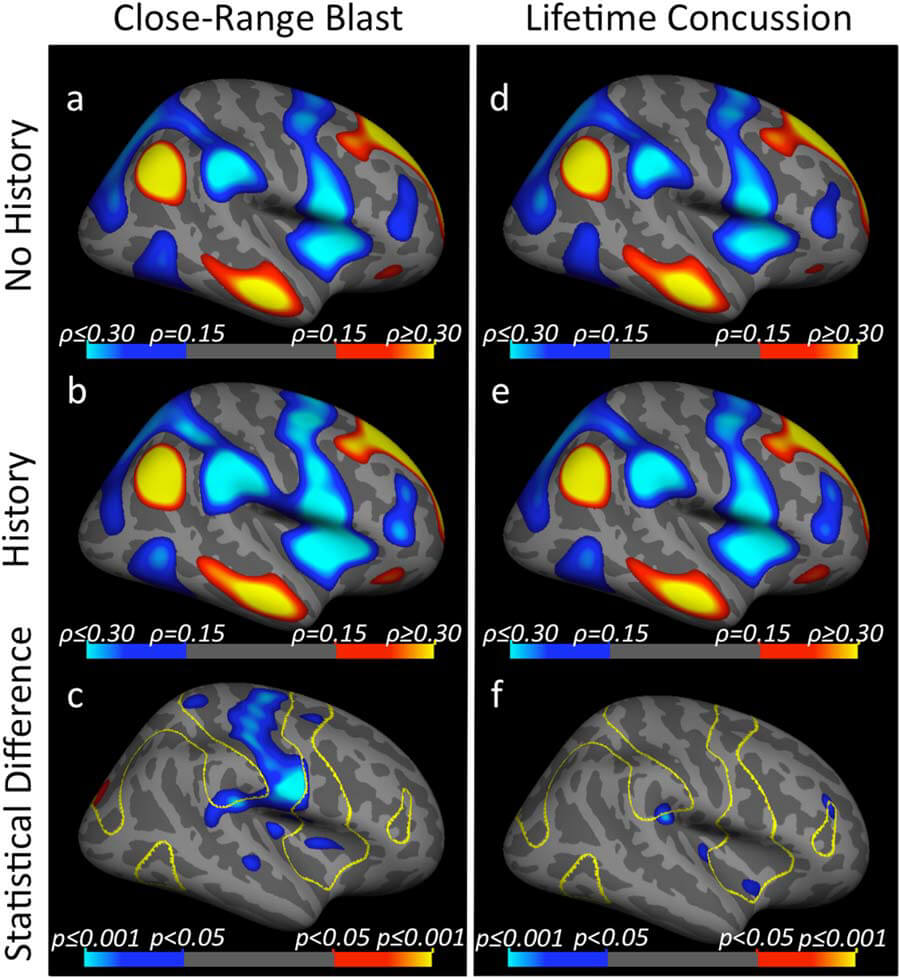
Distance from a blast more accurately predicts persistent changes in the brain, Robinson and the TRACTS team found. Exposure to a blast at less than 10 meters is associated with significant changes in the connectivity between the default mode network and other brain regions, independent of reported mild TBI.
Another study, led by Benjamin Trotter, a TRACTS research assistant, demonstrated that exposure to blasts within 100 meters led to more rapid reduction of white matter tissue integrity, with an increased number of blasts exacerbating the deterioration. The neurodegenerative effects were independent of other comorbidities or TBI status.2
“Concussion symptoms did not drive these results,” explained Regina McGlinchey, PhD, director of TRACTS. “Prior to the Robinson/Trotter research, most funding went into concussion-related blast injuries. These findings indicate we really underestimated the problem caused by blasts.”
In a study recently published in the Journal of the International Neuropsychological Society, Grande set out to determine what cognitive or behavioral effects might be attributed to blast exposure. Of the approximately 600 Iraq and Afghanistan veterans enrolled in the TRACTS Longitudinal Cohort Study, 333 completed a comprehensive neuropsychological evaluation. The assessment included a test of list learning that enabled the researchers to look at performance of different stages of learning, including encoding, retrieval and recognition.3
Participants who reported being within 10 feet of a blast “had a harder time retrieving information. They performed about the same as others in encoding and recognizing,” Grande told U.S. Medicine. “We wanted to make sure that what we were seeing was real. We thought maybe it’s the concussion that’s driving what we see.”
The researchers analyzed the data without veterans with moderate or severe TBI, then looked at the total number of concussions experienced in life. “We found that the issues were not related to total number of concussions; concussion was not what was driving the findings,” Grande said.
The study concluded that “close proximity to detonated blast munitions might impact memory, and veterans exposed to close-range blast are more likely to demonstrate clinically meaningful deficits,” even after adjusting for comorbidities. And, because the veterans had returned from Iraq and Afghanistan several years earlier, the results suggest a chronic impairment.
“How is this going to help me in the clinic?” Grande asked. “How many would I write had actual memory impairment? When we compared the results to normative data, we found that, in the close blast group, the rate of impairment was about 10 percentage points higher.”
While VA clinicians will not have access to a veteran’s performance on the tests five or 10 years before deployment, these results might prompt them to ask about blast proximity when working with a veteran who reports memory issues, she said.
The TRACTS Longitudinal Study should continue to provide additional information on the impact of blasts on cognitive performance. The study has enrolled 600 veterans from Operation Enduring Freedom, Operation Iraqi Freedom and Operation New Dawn since 2010. Of those, 300 have returned for a second round of evaluations, and a third round began in 2016. The TRACTS data repository tracks more than 2,500 variables, including biological, genetic, clinical/neuropsychological/trauma and neuroimaging measures.
“We will see over the long term whether problems get worse, when we run the tests again,” McGlinchey told U.S. Medicine. “We hope that folks having some of the other problems, such as substance use and PTSD, will be getting treatment and those problems will be minimized as time goes on and we can rule out their impact as these veterans get older.”
Some treatments currently being studied for PTSD and sleep disorders, such as trigeminal nerve stimulation, might prove useful for individuals with blast injuries, McGlinchey added.
“Today we have a snapshot,” said Grande. “Now we want a whole movie. Hopefully, we can change the ending for some of our veterans.”
1Robinson ME, Lindemer ER, Fonda JR, Milberg WP, McGlinchey RE, Salat DH. Close-range blast exposure is associated with altered functional connectivity in Veterans independent of concussion symptoms at time of exposure. Hum Brain Mapp. 2015 Mar;36(3):911-22.
2Trotter BB, Robinson ME, Milberg WP, McGlinchey RE, Salat DH. Military blast exposure, aging and white matter integrity. Brain. 2015 Aug;138(Pt 8):2278-92.
3Grande LJ, Robinson ME, Radigan LJ, Levin LK, Fortier CB, Milberg WP, McGlinchey RE. Verbal Memory Deficits in OEF/OIF/OND Veterans Exposed to Blasts at Close Range. J Int Neuropsychol Soc. 2018 Jan 24:1-10.

